As medicine and dentistry continue to evolve and technology advances, patients become more used to minimally invasive surgical procedures with lower morbidity and less postoperative discomfort. Delia Tuttle, DDS, introduces the GumDropTechnique, a new soft-tissue grafting technique that combines minimally invasive incisions with blood derivatives to achieve root coverage and increased keratinized tissue.
We are living in an era in which medicine and dentistry are evolving. As technology drives surgical techniques to become minimally invasive, patients are becoming used to procedures that have lower morbidity and less postoperative discomfort. Dentistry has become part and parcel to that change in the realm of soft-tissue grafting and root coverage procedures. The purpose of this article is to introduce the GumDropTechnique (GDT), a new soft-tissue grafting technique that combines minimally invasive incisions with blood derivatives to achieve root coverage and increased keratinized tissue.
Many root coverage procedures have been described in the literature with varying degrees of success. Autogenous connective tissue grafting remains the gold standard for root coverage and increasing keratinized tissue around natural teeth. This procedure, however, requires a secondary donor site, which can lead to increased pain, morbidity, and limitations in tissue when quadrant or full-arch grafting is needed. Soft-tissue allograft (human cadaver tissue) and xenograft (animal tissue) alternatives have been introduced to overcome these limitations, but the literature has been controversial as to their equality with autogenous connective tissue.
ALSO BY DR. DELIA TUTTLE |Importance of soft tissue in interdisciplinary cases: A case study involving orthodontics, periodontics, dental implants
Biological factors, such as growth factors and proteins, have been introduced as solo or combination agents to increase wound healing and success rates. In addition, minimally invasive surgical techniques have been used with various materials in an attempt to decrease postoperative discomfort. GDT is a technique that encompasses all of the positive benefits of an autogenous, minimally invasive, and biologically enhanced soft-tissue procedure. The surgical procedure for GDT is described below.
Procedure for GumDropTechnique
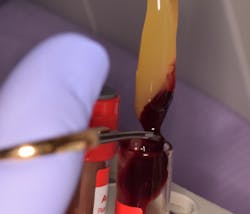
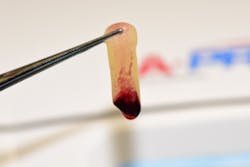
1. Prior to surgery, peripheral blood is collected in 10 ml vials without anticoagulant and immediately centrifuged to 1,300 rpm for eight minutes (figure 1).
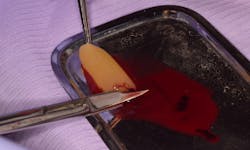
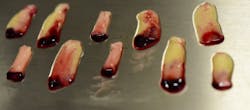
2. After the physiological coagulation, the fibrin clot is separated from the red blood cell component base using scissors and tweezers, and A-PRF membranes are fabricated using the lid of the A-PRF box (figures 2–5).
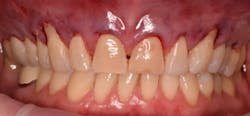
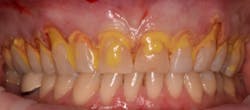
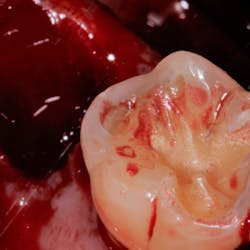
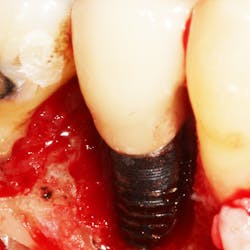
3. Mechanical and chemical root decontamination is performed prior to surgery using scalers, diamond fine burs, and minocycline for a duration of three minutes (figures 6–10). Good oral hygiene is verified.
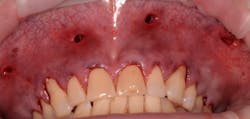
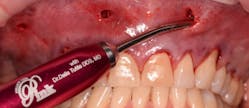
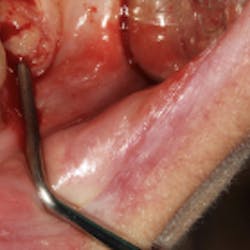
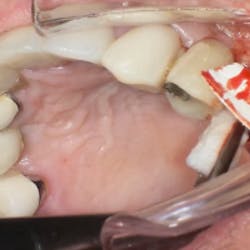
4. The surgical procedure is performed using a small gum-piercing instrument to create holes comparable with a laparoscopic procedure in medical surgeries. Four holes are usually enough to treat the entire arch (figures 11–12).
5. A full subperiosteal flap is then tunneled with appropriate instruments, and multiple A-PRF membranes are introduced inside the elevated tissue (figure 13). The gums are advanced toward the CEJ, and a tension-free flap release is performed and stabilized with sutures.
Coronally advanced flap (CAF) is maintained using an apical mattress suture (figure 14). Glycolon sutures 5.0 or 6.0 are the desired sutures to be able to maintain the flap in close contact with root proximity for at least three to four weeks.
At the end of surgery, another blood draw is required to obtain the injectable I-PRF using 700 rpm for three minutes. The I-PRF liquid from the red layer of RBC will be injected into the surgical side using a syringe and a needle. The growth factors and mesenchymal cells from I-PRF will stimulate the fibroblast growth, and the cells will repopulate the root surface to form new connective tissue attachment.
The growth factors released from platelets and leukocytes will stimulate new vessel growth through VEGF (vascular endothelial growth factor) and FGF (fibroblast growth factor) and will stimulate the PDL to obtain new attachment. The periodontal ligament contains fibroblast cells, epithelial cells, undifferentiated mesenchymal cells, and cementum cells. The success of any grafting procedure depends on the blood supply, and vascularization is key. VEGF and PDGF (platelet derivative growth factor) are responsible for angiogenesis. PDGF is also a mitogen for cells of mesenchymal origin, including fibroblast.
The tension-free flap reattachment on the root surface will be assisted by two main components of this technique: growth factors and the apical mattress suture. Moreover, the fibrin matrix shows mechanical adhesive properties and functions as fibrin glue, which maintains the flap in a stable position, induces vascularization, reduces necrosis, and promotes root coverage.
Conclusion
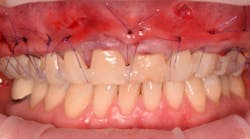
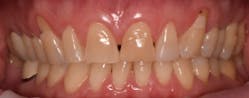
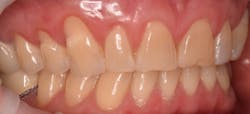
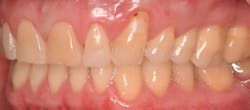
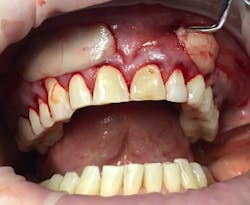
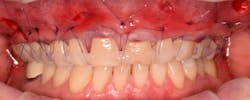
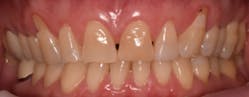
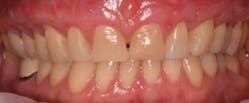
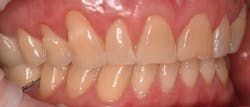
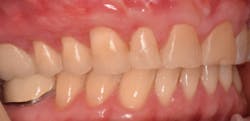
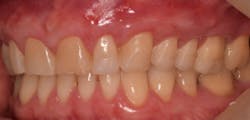
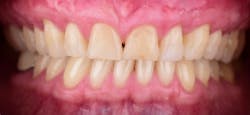
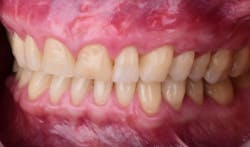
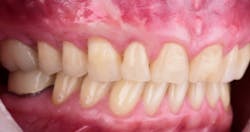
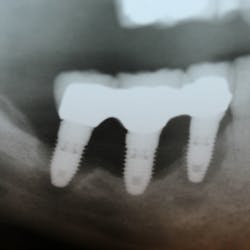
This new biological approach involving blood derivatives A-PRF and I-PRF combined with precision minimally invasive surgery for root coverage demonstrates faster healing without the need of a donor site. The morbidity of GDT is decreased and patient case acceptance is higher compared with traditional grafts. Before-and-after pictures are shown below (figures 15–22).