Give me six hours to chop down a tree and I will spend the first four sharpening the axe. — Abraham Lincoln
Contrary to a common belief of patients and even of some dentists, dental implant therapies are not everlasting. If implantology continues to grow at its current pace, the general practitioner in the future will have to face implant therapy failures and complications on a daily basis. Still, today, we encounter a growing number of clinical situations in which an individual patient has received different implants with different angulations, from different oral surgeons with different criteria for success.
RELATED | Vertical ridge augmentation: Using a titanium-reinforced high-density PFTE membrane
RELATED |'My implant is too shallow and now I'm getting food stuck between my teeth'
Mrs. Y is a 61-year-old woman, with no particular health problem when she comes to our practice, in January 2013, seeking help to escape from an implant rehabilitation dead end.
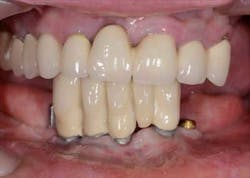
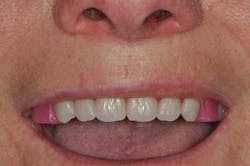
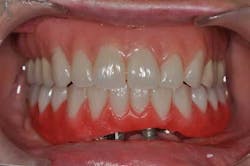
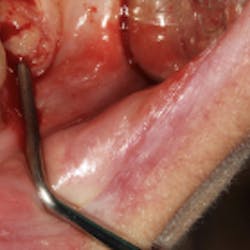
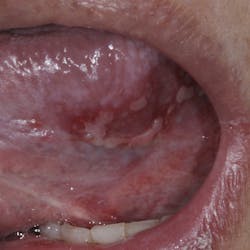
Figs. 1a and 1b: Initial situation of the 61-year-old female patient
Maxillary arch: crown and bridgework collapsing from 3 through 11 and the missing teeth in the upper left are replaced with a partial denture. All the remaining teeth are doomed to extraction.
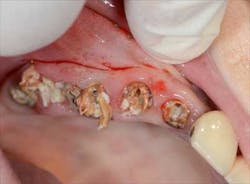
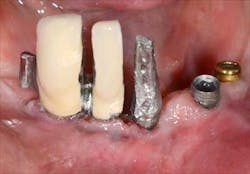
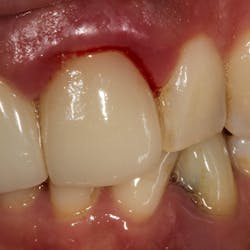
Fig. 2: Remaining teeth in the upper right
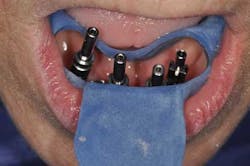
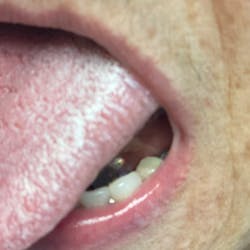
Mandibular arch: the lower jaw is fully edentulous. Initially, according to the patient, an implant-supported five-unit bridge (23 to 27) was made on four implants (Alphabio®) placed in 2007. Tooth 22 was present at the time and a removable partial denture replaced the bilateral posterior missing teeth.
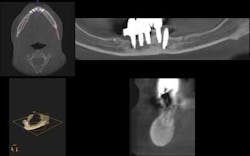
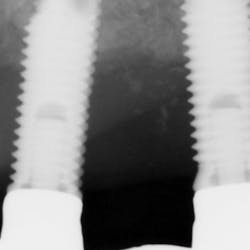
Then, in January 2012, tooth 22 was extracted and a second implant specialist placed a new implant (Zimmer Dental®) to replace it. The GP decided to use a Locator® attachment system on this new implant and have the existing denture stabilized over it, without paying any attention to the collapsing situation of the upper right.Fig. 3: CT scan shows the existing implants positions and the bone volume available
A few months after this treatment phase, the patient is still unable to chew comfortably. The lower denture is now hurting and she notes a bad odor coming out of the now moving upper right teeth. Even more sadly, she can’t find a dentist able to get her out of trouble.
Step 1: What is it?
Before you make any move, the first thing you want to know is the precise reference of each dental implant in place. Our patient was asked to contact both of the implant specialists and collect the following data:
- Implant brand
- Implant diameter
- Implant length
- Implant connection type
- Implant trackability sticker
It is sometimes difficult, if not impossible, to collect this information (vanished dentist, loss of records, bankrupted brand). If this is the case, you only have two solutions left:
- Use your professional network and/or the Internet (http://whatimplantisthat.com) to send radiographs of the implants and hope to get some help that way. Be aware that this solution is rather unpredictable.
- Consider removing the implant(s) right away.
Step 2: Implant prosthetic equipment
Now that you have collected the implant information, you need to examine the brand product catalogue (on the Internet) and browse the prosthetic component available.
We suggest that you avoid the primary instinct of calling the brand technical support for help. Take time to pick up and study the implant system(s) characteristic(s) for a few minutes. In case you need help from the tech-com support, you will be ready to clearly address your problem and remain critical regarding the solutions offered to you.
The equipment you’re looking for is impression equipment for your implants: conical abutments (if needed), transfer copings, transfer coping screws, implant replicas, and healing abutments eventually.
Also ask yourself if your own screwdrivers and torque wrenches are compatible with the implant system(s) you are dealing with.
Finally, keep an eye on the costs.
Step 3: Prosthetic planning
Now that we can take an impression of these implants, we need to build a treatment plan in order to make sure that the position of the existing implants will permit the making of a prosthesis able to satisfy the patient’s functional and esthetic needs.
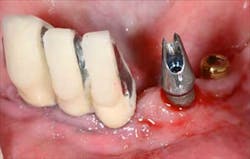
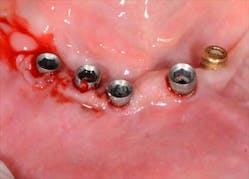
Figs. 4a, b, c: Removal of the implant prosthesis
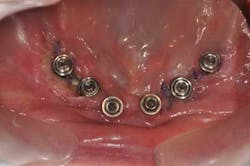
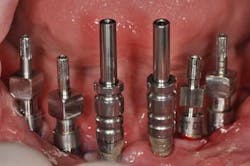
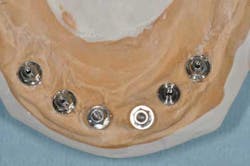
Fig. 5: The different conical abutments ordered
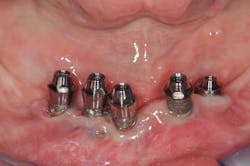
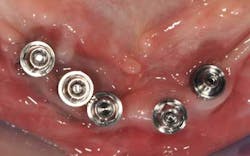
Fig. 6a: Conical abutments, buccal view
Fig. 6b: Conical abutments, occlusal view
Fig. 7a: Transfer copings
Fig. 7b: The positioning of the transfer copings already shows inadequate implant positions
Fig. 7c: Transfer coping placement on site 26 is impossible: this implant will have to be removed or submerged
Fig. 8: An impression is taken with a custom tray
Figs. 9a, b, c: A wax-up is made in the laboratory …
Figs. 10a, b: … and clinically tested for esthetic and functional evaluation. In this case, the wax-up has been quickly turned into a provisional maxillary complete denture.
At this point, the final treatment plan must be approved and consented by each of the following:
- Restorative dentist
- Lab technician
- Implant surgeon
- Patient
In order to do so, each of these issues must be addressed:
- Conservation/removal/submersion of the existing implants
- Need for new implant(s) placement
- Type of prosthetic design: implant retained removable, screw-retained, cement-retained …
- Benefits, drawbacks, risks, costs
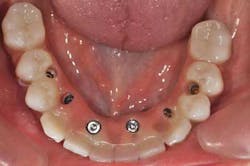
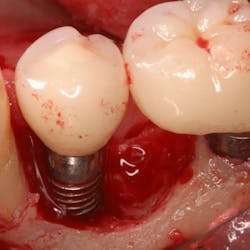
Fig. 11: For a better prosthetic outcome, the implants in site 26 and 27 have been extracted and replaced with two Biomet 3i® implants.
Fig. 12: A new implant impression is taken
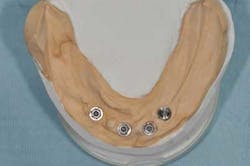
Fig. 13a, b: The new master cast shows the modified implant situation
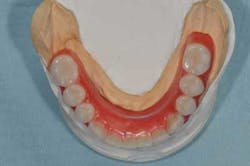
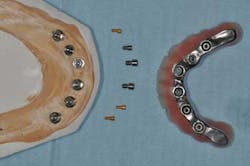
Fig. 14: Hybrid screw-retained mandibular prosthesis
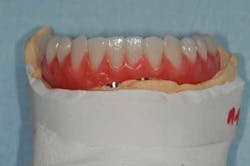
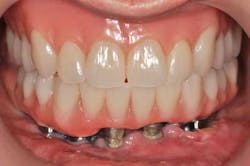
Fig. 15a, b: Final result (removable complete denture on the maxillary)
Complications and failures in implant dentistry are growing concerns. The worse of them all are the treatment planning errors. Successful management of these sensitive situations requires time for systematic and comprehensive analysis of the:
- Clinical parameters (biological as well as psychological)
- Technical performances of the different implant systems in presence
- Laboratory technical possibilities
- Interventional risks, potential hazards, and costs
All surgical procedures by Dr. Thierry DeGorce.