While most oral conditions can be resolved with dental therapy, there are also many systemic diseases that manifest themselves in the oral cavity, thus requiring the consult of a medical physician. Dr. Scott Froum, editorial director of Perio-Implant Advisory, addresses five of the most common questions dental patients ask about pathology in the mouth and shares answers you can use in your practices.
A COMMON MISCONCEPTION in medicine is that the mouth is disconnected from the rest of the body when dealing with disease. On the contrary, the mouth can be a window into the systemic health of an individual. Most oral issues are confined to the mouth and can be resolved with dental therapy. However, oral manifestations of systemic disease are prevalent and may require the consult of a medical physician.
Listed below are some common questions patients ask their dentists about pathology found in the mouth and the answers to those questions.
No 1: Could changes in my gums be a sign of a bigger issue?
Changes in gum tissue, texture, tone, and inflammatory state (i.e., bleeding) are often signs of poor oral hygiene and the need for a professional cleaning.
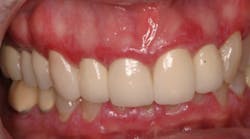
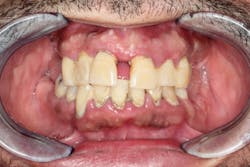
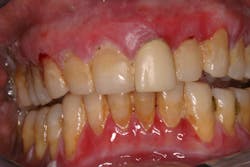
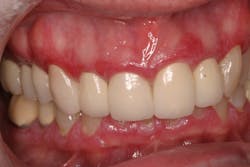
However, in some cases, these symptoms may indicate a change in health status, such as the development of diabetes (figure 1); changes in the immune system; pregnancy; blood dyscrasia (figure 2), including leukemia, neutropenia, and conditions that affect platelets; or a nutritional deficiency in vitamin B3 and/or vitamin C.
Figure 1: Patient with diabetes
Figure 2: Patient with neutropenia
No. 2: Could pain or discoloration of teeth mean something else is wrong?
There are two causes of tooth discoloration: extrinsic and intrinsic stain.
Extrinsic stain is usually due to common causes. Brown stains are a result of food and drinks such as coffee, tobacco, red wine, and chocolates. Green and orange stains can be due to tartar buildup.
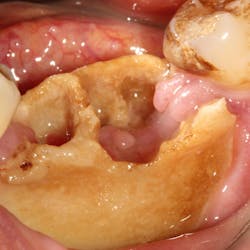
Intrinsic stain comes from within the tooth. Grayish-blue to brownish-yellow stains can be from tetracycline staining, caused by exposure of the tooth to the antibiotic when the tooth was developing. White patches on the tooth that look chalky can indicate too much exposure to fluoride, or what is known as fluorosis. Grayish-black stains can suggest cavities from within the tooth. If the pulp or nerve of the tooth dies, the tooth can turn black or brown. If the tooth sustains trauma and the pulp begins to bleed, the tooth can turn black (figure 3).
Figure 3: Patient with tooth discoloration due to trauma
No. 3: Could tongue pain or having a strange taste in my mouth be cause for worry?
Inflammation of the tongue is known as glossitis, and pain of the tongue is known as glossodynia. The most common causes of pain in the tongue can be from canker sores (also known as aphthous ulcers) or cold sores (herpes); dehydration; dry mouth; fever (sickness); or the Candida infection (commonly known as thrush). Thrush can appear as a white lesion that bleeds when scraped or as a red, roundish lesion.
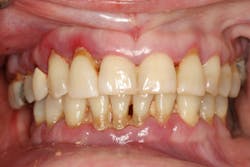
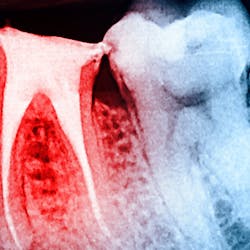
Pain or burning of the tongue can also indicate a vitamin deficiency, such as B12 pernicious anemia (figure 4), and/or vitamins B2, B3, B6, and B9. Other pains in the tongue can be caused by more serious conditions such as oral cancers, which can appear as red and/or white lesions. If any sore does not go away within two weeks, consult your dentist for an examination.
Figure 4: Patient with pernicious anemia from vitamin B12 insufficiency
Complete loss of taste is called ageusia, partial loss of taste is called hypogeusia, and a distorted sense of taste is called dysgeusia. The most common cause of strange taste is due to medications. The most common peculiar taste is a metallic taste, which is associated with some forms of antibiotics, antihistamines, antifungals, antipsychotics, blood pressure medications, diabetes medications, seizure medications, and Parkinson’s disease medications.
Other more common conditions that can change one's taste are dry mouth, colds or flu, smoking, loss of smell, and nutritional deficiencies (vitamin B12 and zinc)
No. 4: Are there any other small symptoms that could indicate larger problems? If so, what are they?
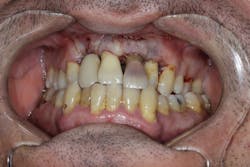
Koplik's spots appear two to three days before the measles rash and look like clustered white lesions on tissues near the lower first and second molars. They are usually the first signs of measles and manifest in the oral cavity.Other autoimmune diseases—such as pemphigoid and pemphigus (figure 5)—can appear as inflamed gum tissue and may be signs of other more serious conditions.
Most of the time the condition you have is either cavities or periodontal disease. However, on that rare occasion when your oral pathology is not due purely to dental disease and your sores do not go away after two weeks, be sure to consult with a dental professional.
Figure 5: Patient diagnosed with pemphigus
No. 5: Is bad breath caused by other oral health issues?
Bad breath—also known as halitosis—can be caused by oral health issues, systemic medical problems, and/or a combination of both. It is estimated that 80% of halitosis is caused by oral diseases such as bacteria from cavities and bacteria found in the deepened sulcus of the gingival tissue, dorsum of the tongue, and saliva. Certain bacteria in the oral cavity that are responsible for a breakdown of products that contain volatile sulfur compounds (VSCs) are most known as the causal agents for halitosis. The VSCs most associated with halitosis are methyl mercaptan, hydrogen sulfide, and dimethyl sulfide.
Additional oral causes of halitosis (usually the causal agent of bad breath 20% of the time) can be from issues such as gastroesophageal reflux disorder (GERD), sinusitis, metabolic disorders, respiratory disorders, and immunologic disorders.