Probiotic overuse and misuse: How to determine what probiotic your dental patient needs
Probiotics are live microorganisms that provide health benefits when consumed, typically by improving or restoring gut flora. Probiotics are known to provide various health benefits, such as balancing the digestive system, improving mental health disorders, lowering cholesterol levels, and enhancing overall immunity. They also aid in lowering symptoms of gastrointestinal (GI) diseases, such as yeast infections, diarrhea, irritable bowel syndrome, eczema, lactose intolerance, urinary tract infection, and constipation.1
Probiotics have been used in the dental field to repopulate the oral cavity with good bacteria after periodontal debridement of periodontal pathogens.2 They have also been used to treat patients with halitosis, black hairy tongue, thrush (candida), and/or high cavity rates.3 Despite their positive health outcomes, if overused and/or misused, the risks of probiotics can outweigh their benefits.
Probiotic overuse
The overuse and indiscriminate administration of probiotics have reached epidemic proportions. The global probiotic market size has reached $57.1 billion in 2023 and is assessed to grow at a compounded annual growth rate of 8.7% from 2024 to 2032. By the end of 2032, the probiotic consumer market is expected to exceed $91.4 billion.4
The adage too much of a good thing is a bad thing holds true with probiotic use. Unfortunately, simply taking a probiotic without direction or without knowing what bacteria you are deficient in can cause systemic problems.
For example, one type of bacteria commonly found in over-the-counter probiotics, Lactobacillus, has been associated with an increase in D-lactic acid and has caused SIBO (small intestinal bowel overgrowth) in certain patients.
Other studies have shown that overreliance on probiotics can cause brain fog, poor concentration, short-term memory problems, and metabolic acidosis.5 The authors of this study concluded that probiotics should contain strains of bacteria that are patient-specific and should be treated like a medication, not a supplement.
Probiotic misuse
Although there are numerous brands of probiotic supplements (figure 1), many contain a limited number of bacterial strains, primarily from the groups Lactobacillus, Bifidobacterium, and a few others. Patients who take probiotics without knowing which strains they need can do more harm than good.
For instance, concentrated doses of a few strains of bacteria (e.g., Lactobacillus casei) can upset the balance in the gut inadvertently by creating a form of dysbiosis that comes from having too much of a good bacterium, which decreases the more important factor of microbiome diversity.
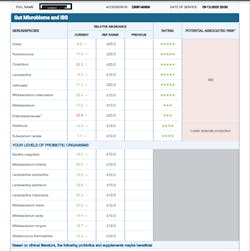
Directed probiotic use should include oral saliva and stool testing. This will determine the patient’s oral and gut microbiome and ascertain what bacteria strains are or are not needed (figure 2). Based on this information, the clinician can then determine what, if any, probiotic is needed and how it needs to change over time to support the evolving microbial flora. In other words, one type of probiotic should not be taken ad infinitum, and focus should be placed on increasing the diversity of microbial flora.
How to determine what probiotic is needed
- Take a thorough patient history, including medical conditions, medications, signs and symptoms, nutritional history, and current supplementation.
- Oral saliva (Oral DNA Labs) and stool tests (Vibrant Wellness Labs) should be taken to ascertain the oral and gut microbiome, looking for the presence of possible dysbiosis. Research studies may be available that can test gut microbiome for free (Zoe PREDICT Research Study).
- Collaborate with a professional (Meraki Integrative) or a professional company (Floré) that will customize a probiotic program tailored to the needs of the individual patient.
- In addition to probiotics, focus on prebiotic and postbiotic foods (fiber and low-sugar fermented foods) that increase microbial diversity.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Derwa Y, Gracie DJ, Hamlin PJ, Ford AC. Systematic review with meta-analysis: the efficacy of probiotics in inflammatory bowel disease. Aliment Pharmacol Ther. 2017;46(4):389-400. doi:10.1111/apt.14203
- Canut-Delgado N, Giovannoni ML, Chimenos-Küstner E. Are probiotics a possible treatment of periodontitis? Probiotics against periodontal disease: a systematic review. Br Dent J. 2021. doi:10.1038/s41415-021-3624-5
- Homayouni Rad A, Pourjafar H, Mirzakhani E. A comprehensive review of the application of probiotics and postbiotics in oral health. Front Cell Infect Microbiol. 2023;13:1120995. doi:10.3389/fcimb.2023.1120995
- Global probiotics market outlook. EMR Expert Market Research. https://www.expertmarketresearch.com/reports/probiotics-market
- Rao SSC, Rehman A, Yu S, Martinez de Andino N. Brain fogginess, gas and bloating: a link between SIBO, probiotics and metabolic acidosis. Clin Transl Gastroenterol. 2018;9(6):162. doi:1038/s41424-018-0030-7
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.
Brigitte Rizzo, NP
Brigitte Rizzo, NP, is a nurse practitioner who graduated with honors from the State University of New York at Stony Brook, School of Medicine in 2002, and has been practicing internal medicine for more than 20 years. She has multiple certifications in the integrative wellness field with licenses in multiple states. She is currently in private practice at Meraki Integrative and Wellness at 120 Remington Blvd., Ronkonkoma, NY 11779 and is cofounder of the Metatron Miracles Recovery and Rehab Center in Naples, Florida.
Updated September 6, 2022