Localized aggressive periodontitis: All-On-4 oral rehabilitation case report
Patient: A 20-year-old African American female
Diagnosis and treatment: All-On-4 oral rehabilitation
The American Academy of Periodontology, as of 1999, has reclassified periodontal disease, which affects young individuals. (1) Classifications include:
- Dental plaque-induced gingival diseases
- Chronic periodontitis
- Aggressive periodontitis
- Periodontal diseases as a manifestation of systemic disease
- Necrotizing ulcerative diseases
The current case report describes a young African American female diagnosed with localized aggressive periodontitis (LAP) at approximately puberty and developing into a generalized form of the disease as the patient entered late adolescence. This aggressive form of periodontal disease may manifest itself in both the primary and permanent dentitions.
Many years ago, aggressive periodontitis in the primary dentition was classified as localized prepubertal periodontitis (LPP) and localized juvenile periodontitis (LJP) in the permanent dentition.
ADDITIONAL READING |Increasing dental case acceptance through the use of salivary diagnostics
Localized aggressive periodontitis affects the first molar teeth and/or incisors.
The recommended treatment of scaling, root planing, and antibiotic therapy, along with surgical intervention if deemed necessary, will curtail the progression of the aggressive infection.
The most significant aspect of this current investigation, and the most unfortunate, is that the disease progression continued into the generalized form of aggressive periodontitis three years following initial therapy. Despite three-month maintenance recall therapy, use of antibacterial therapy, and implementing doxycycline hyclate (20 mg) twice daily, the disease progression did not slow or stop.
ADDITIONAL READING |Understanding and managing peri-implant bone loss
The following case history describes the diagnosis and subsequent clinical treatment rendered to this young adolescent, who subsequently underwent complete edentulation and an All-On-4 approach for oral rehabilitation. (2)
Case report
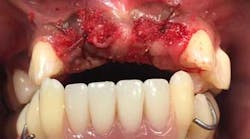
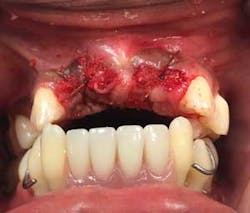
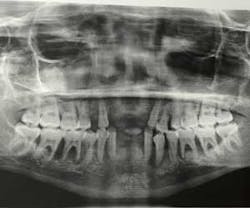
A 17-year-old, African American female, well nourished and otherwise healthy, was referred for bone loss associated with teeth Nos. 21, 22, 23, 24, 25, 27, and 28 (figures 1 and 2).
The patient underwent full-mouth periodontal and radiographic examination. A blood chemistry profile and complete blood count was advised and obtained to eliminate any systemic abnormalities.
At the initial visit, the patient was prescribed 250 mg tetracycline HCl three times daily for a 14-day period. Four weeks later, scaling and root planing ensued under local anesthesia and 100 mg doxycycline HCl was prescribed once daily for three weeks. The blood chemistry profile returned generalized findings within normal limits. Most concerning would be the coincidental finding of juvenile diabetes, blood disorders, or any other type of bone-resorbing disorders.
Following two consecutive, three-month recall procedures, assessing patient compliance, and evaluating oral home care, periodontal probing depths were measured at a similar level as baseline. A treatment plan was presented to surgically debride all bony defects, plane all root surfaces and bone graft defects, which were found to be vertical in nature.
All surgical sites were sutured to attempt primary closure, and the patient was given specific postsurgical hygiene instruction. The patient was prescribed 20 mg doxycycline hyclate (continuing for a nine-month period), 800 mg ibuprofen three times a day for discomfort, and 0.12% chlorhexidine.
The patient returned at seven days postsurgery. Gingival tissues were found to be healing favorably without significant postoperative complications or thermal sensitivity. The patient was advised again to remain on 20 mg doxycycline hyclate and return in a one-month period to undergo a periodontal recall maintenance.
During the next 30 months, the patient underwent 10 periodontal recall maintenance visits. The patient demonstrated favorable home care with minimal plaque and calculus deposits. A fluoride varnish was applied at every recall to reduce and control root sensitivity. The patient was prescribed 20 mg doxycycline hyclate to aid in reduction of alveolar bone resorption and a consistent three-month recall was strongly advised.
Six months postsurgery, a recommendation was made to the patient to remove the lower incisor teeth—Nos. 23, 24, 25, and 26—due to increased mobility and discomfort upon chewing. A lower anterior temporary partial was provided (figure 3).
Over the following year, a moderate amount of plaque and calculus was observed and home care began to fail. The patient reported difficulty with chewing, and switching to a soft food diet did not seem to be helpful. Periodontal recall maintenance continued on a three-month basis.
In the next year, the patient described discomfort with tooth No. 5 and generally presented with swollen appearance to the gingiva. Amoxicillin and metronidazole was prescribed to help reduce infection and swollen tissues. The patient was advised to practice safe sex, using protection while taking the antibiotic cocktail. Teeth Nos. 7, 8, 9, and 10 were scheduled to be removed, and a maxillary temporary partial was fabricated for tooth replacement.
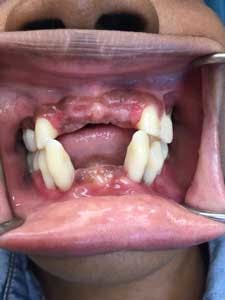
Upon returning for the above tooth removal, tooth No. 5 self-avulsed and the other teeth were removed and a temporary partial placed (figures 4 and 5).
Approximately, two-and-a-half years into active periodontal treatment and maintenance therapy, the patient and the authors discussed removal of all remaining teeth and rehabilitation of the mouth with the All-On-4 (AO4) approach (figure 6).
At this time, the patient, having an active lifestyle as a student and working her way through school, wished not to be distracted by continuous tooth problems involving infections and loss of teeth. An appointment was then scheduled for a four-hour visit under I.V. sedation and local anesthesia to perform the AO4 oral rehabilitation.
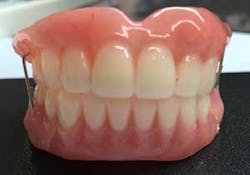
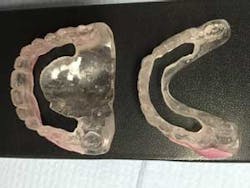
Of course, proper records were obtained in order to fabricate the temporary provisional prosthesis (figure 7), upper and lower, to provide proper function, esthetics, and easy conversion.
A panoramic radiograph (figure 8) and cone beam CT (CBCT) scan were obtained for evaluation of alveolar bone height and width and all sinus and mental foramen positions.
Due to the aggressive bone loss of the periodontal disease type, a more conservative approach was possible and bone removal was carefully planned if it would become necessary.
The AO4 approach began with measuring the occlusal vertical dimension (OVD), by marking to spots on the chin and nose, which would aid in evaluating the final OVD after conversion of the provisional prosthesis.
The mandibular and maxillary arches were completely edentulated, and all second and third molar sockets were sutured closed.
Surgical stents (figure 9) mimicking provisional teeth were placed in position to assess the need for any alveolar bone reduction. Alveolar bone was slightly reduced associated with each canine eminence and mandibular anterior crestal ridge, approximately 2 mm.
Due to the aggressive nature of the disease process, the previously resorbed alveolar bone was very adequate for placement and conversion of the mandibular and maxillary prosthesis.
In the maxilla and mandible, distal implants were placed at proper 30- to 45-degree angles, avoiding sinus perforation and trauma to the mental foramen, respectively.
Anterior implants were placed straight, with the exception of the maxillary left implant placed to avoid a previously developed periodontal defect. All implants were grafted with a combination of mineralized and demineralized human bone allografts, and remaining sockets bone-grafted to enhance alveolar ridge preservation (figure 10). (2)
Transmucosal abutments or multiunit abutments were then placed onto dental implants, using straight, 17-degree, or 30-degree angulation to conform to the conversion prosthesis for proper stability and torquing.
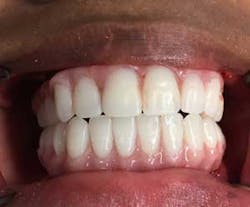
Provisional prostheses were then positioned and upon proper stability, function, and cosmetic appearance were torqued to 15 Ncm. At this point, the occlusion was evaluated; posterior occlusion was adjusted to be extremely light, and occlusion associated in the anterior region carried more inter-arch load (figure 11). (2)
A soft diet along with postoperative instructions was stressed, particularly during the first six weeks of healing.
Maintenance
Maintenance on a three- to four-month basis was strongly advised to aid the patient in proper home care and healing. Panoramic radiographs are periodically obtained to continue to evaluate bone support of the supporting dental implants.
The All-On-4 protocol on this young patient is timeless, yet perhaps questionable.
The authors strongly believe that with the aggressive nature of her periodontal infection and associated types of bacteria, pathogenic to this aggressive disorder, complete tooth removal and rehabilitation with this protocol will provide this young patient with confidence and enthusiasm about living her life without dental complications (figure 12).
Acknowledgment: The authors wish to thank BioHorizons Implant Company for providing implant parts and implant connections for the All-On-4 procedure pro bono.
Alphonse Gargiulo, DDS, MS,is in private practice at Park Dental Specialists in Chicago, Illinois. You may contact him at [email protected].
Rachel Degen, RDH,is a hygienist at Park Dental Specialists in Chicago, Illinois.
Mark Val, CDT,is the owner of Prestige Dental Laboratory in Chicago, Illinois.
References
1. Armitage G. Development of a classification for periodontal diseases and conditions. Ann Periodontol. 1999;4:1–6.
2. Malo P, Nobre Mde A, Petersson U, Wigren S. A pilot study of complete edentulous rehabilitation with immediate function using a new implant design: Case series. Clin Implant Dent Relat Res. 2006;8:223–232.
3. Ho ChK, Javonvic S. The All-On-4 concept for implant rehabilitation of an edentulous jaw. Compend. 2014;35:255–259.
4. Kim Y, Ol T-J, Misch C, Wang H. Occlusal considerations in implant therapy: Clinical guidelines with biomechanical rationale. Clin Oral Implant Res. 2005;16:26–35.