Perio-Implant Advisory JOMI Clinical Pearls: Discussions on zirconia versus titanium implants, peri-implantitis, and dental implant geometry
JOMI Clinical Pearls is a regular column in Perio-Implant Advisory that discusses articles from The InternationalJournal of Oral and Maxillofacial Implants (JOMI)—the official journal of the Academy of Osseointegration (AO)—as reviewed by a member of the Academy’s Young Clinicians Committee (YCC). Quintessence Publishing publishes JOMI. Today’s studies are all pulled from Volume 30, Number 4, 2015.
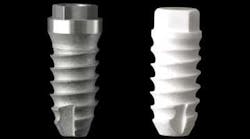
The first article I reviewed is titled “Comparison of Clinical and Histologic Outcomes of Zirconia Versus Titanium Implants Placed in Fresh Sockets: A 5-Month Study in Beagles.” This group of researchers from Spain compared the histologic outcomes obtained when titanium (Ti) and zirconia (Zr) implants were placed in fresh extraction sockets in an animal model. Eight dogs received two titanium and two zirconia implants in the distal sockets of the third and fourth premolars, placed at bone level and in a two-stage approach. After five months, nine of 32 implants failed, with a higher survival rate for Ti implants. Difference in surface roughness, the lack of oral hygiene, and the animal’s diet were identified as possible causes for a higher failure rate. Bone-implant contact and bone loss were similar in remaining Zr and Ti implants. The interest in zirconia as an alternative to titanium has long roused interest among researchers. More recent studies are suggesting zirconia as a viable alternative to conventional titanium implants, calling for further research to build consensus.
ADDITIONAL READING |Perio-Implant Advisory JOMI Clinical Pearls: Analyzing techniques for maxillary implant placement success
The second article is titled “Microbiologic and Clinical Findings of Implants in Healthy Condition and with Peri-Implantitis.” In this cross-sectional study, the authors collected samples for microbiologic analysis from three locations associated with dental implants: the peri-implant sulcus, inside the implant connection, and the gingival sulcus of adjacent teeth. A quantitative real-time polymerase chain reaction PCR assay was carried out for total bacterial count and for 10 pathogens. Orange complex species (Prevotela intermedia, Peptostreptococcus micros, Fusobacterium nucleatum) were most prevalent in all sites for both groups, and prevalence values were higher for the peri-implantitis group. In general, absolute loads and total bacterial counts were higher for the peri-implantitis group. Differences in prevalence between groups were more marked inside the implant connection than in the peri-implant sulcus, suggesting the implant connection as a potential microbial reservoir for peri-implant disease. Peri-implantitis is one of the hottest topics in implant dentistry today. Interest in this disease process is such that it has warranted a number of special supplement issues, including a thematic abstract review published in IJOMI in 2013.
The third article is titled “The Effect of Interimplant Distance on Peri-Implant Bone and Soft Tissue Dimensional Changes: A Nonrandomized, Prospective, 2-Year Follow-up Study.” In this clinical study, the authors evaluate hard- and soft-tissue changes around adjacent implants placed at different horizontal interimplant distances. The patients were divided into three groups: In group A, the implants were placed at 2 millimeters (mm) apart, in group B 3 mm, and at 4 mm or more in group C. The results failed to demonstrate that interimplant distance significantly influenced marginal and midproximal bone level changes. For this particular study, implants with an internal conical connection and platform-switch were used. This type of configuration has shown to be more effective in the maintenance of peri-implant bone levels in several studies. Advances in dental implant geometry and configuration have led to more favorable peri-implant tissue response, improving the outcomes of dental implant therapy.
ADDITIONAL READING | Understanding and managing peri-implant bone loss
The areas I address above are important to all of us in our field. I am a member of AO because it allows me to have access to a number of resources that I can use in my daily practice. I read JOMI to keep up-to-date with the latest research, keep up with my peers, and continue to learn. I attend the annual meeting to learn new things and to see my friends and colleagues. I am also involved with two committees, and I enjoy the committee service, which allows me to interact with experienced and well-renowned clinicians.
One of the many benefits of being an AO member is an automatic JOMI (bimonthly) subscription.
The 31st Annual Meeting is set for February 17–20, 2016, in San Diego. You can register to attend at www.osseo.org. Follow AO on Facebook and Twitter using #AOSanDiego to stay up-to-date.