Perio-Implant Advisory JOMI Clinical Pearls: Photofunctionalization in bone generation, sinus augmentation and composite bone grafts, peri-implant tissue stability
JOMI Clinical Pearls is a regular column in Perio-Implant Advisory that discusses articles from The InternationalJournal of Oral and Maxillofacial Implants (JOMI)—the official journal of the Academy of Osseointegration (AO)—as reviewed by a member of theAcademy’s Young Clinicians Committee (YCC). Quintessence Publishing publishes JOMI. Today’s studies are all pulled from Volume 31, Number 1, 2016.
ADDITIONAL READING |Perio-Implant Advisory JOMI Clinical Pearls: Discussions on zirconia versus titanium implants, peri-implantitis, and dental implant geometry
In particular, the authors addressed the bone generation capability of titanium mesh to (1) fill a gap and (2) extend from the surface over a distance by establishing three-dimensional bone profiling. The titanium mesh (0.2 mm thickness) used in this study was made of commercially pure grade-2 titanium and had hexagonal apertures (2 mm width). Photofunctionalization was performed by treating titanium mesh with UV light for 12 minutes using a photo device immediately before use. Untreated or photofunctionalized titanium mesh was placed into rat femurs, and bone generation around titanium mesh was profiled using three-dimensional microcomputed tomography (micro-CT). A set of in vitro experiments was conducted using bone marrow-derived osteoblasts.
The results showed that photofunctionalized titanium mesh surfaces were characterized by the regenerated hydrophilicity and significantly reduced surface carbon. Bone generation profiling at week three of healing showed that the hexagonal apertures in photofunctionalized mesh were 95% filled, but they were only 57% filled in untreated mesh, particularly with the center zone remaining as a gap. Bone profiling in slices parallel to the titanium surface showed that photofunctionalized titanium mesh achieved 90% bone occupancy 0 to 400 μm from the surface, compared with only 35% for untreated mesh. Bone occupancy remained as high as 55% 800 to 1,200 μm from photofunctionalized titanium mesh surfaces, compared to less than 20% for untreated mesh. In vitro, photofunctionalized titanium mesh expedited and enhanced attachment and spread of osteoblasts, and increased ALP activity and the rate of mineralization.
The authors concluded that photofunctionalization not only increased the breadth but also the 3-D range of osteoconductivity of titanium mesh, enabling space-filling and far-reaching osteoconductivity.
ADDITIONAL READING |Perio-Implant Advisory JOMI Clinical Pearls: Analyzing techniques for maxillary implant placement success
The second article is titled “Dimensional Changes Following Lateral Wall Sinus Augmentation Without Concomitant Implant Placement Using a Composite Bone Graft.” The severely atrophic posterior maxilla usually requires lateral wall sinus augmentation to enable proper placement of dental implants. This procedure is now commonly employed in the dental practice with high predictability and very good surgical outcomes. Nonetheless, some dimensional loss of the bone graft may occur during the healing period and thereafter.
The purpose of this study was to evaluate changes in sinus dimensions immediately postoperatively and one year later using a composite of bovine-derived xenograft and autogenous bone for lateral bone augmentation of the maxillary sinus. Patients who underwent lateral wall sinus augmentation procedures without concomitant implant placement were considered for this retrospective analysis if they had three consecutive panoramic radiographs: pretreatment (T0), immediately after lateral wall sinus augmentation (T1), and approximately one year postoperatively (T2). Eighteen subjects ages 47 to 69 years were included.
The surgical protocol included grafting with a composite of bovine-derived xenograft and autogenous bone (9:1 ratio). Digital panoramic radiographs were transferred into measurement software, and the following measurements were performed: (1) vertical distance from the alveolar crest to the height of the augmented material, (2) sagittal area of the grafted area, and (3) vertical distance from the alveolar crest to the roof of the maxillary sinus.
The results showed that the mean overall sinus sagittal area was 1,330 ± 481 mm2 prior to the grafting procedure, when it decreased to 858.2 ± 436 mm2 (range, 380.7 to 2,134 mm2) immediately postoperatively (P = .0035) and remained stable at one year (mean, 882.2 ± 384 mm2, P > .05). Similarly, the overall area of the grafted material at the time of surgery was 468.3 ± 208 mm2 and was only slightly reduced at one year (422.2 ± 193 mm2). The midsagittal graft height at T1 (mean, 20.67 ± 4.5 mm) was insignificantly and minimally reduced at one year (mean, 19.35 ± 4.9 mm).
The authors concluded that the linear dimensions of composite bone-derived xenograft/autogenous bone grafts following lateral wall sinus augmentation exhibited minimal changes during the eight- to 12-month healing period.
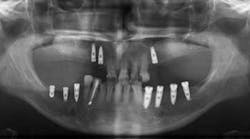
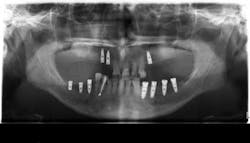
The third article is titled “Peri-implant Hard and Soft Tissue Stability in Implants Placed Simultaneously Versus Delayed with Intraoral Block Bone Grafts in Horizontal Defects: A Retrospective Case Series Study.” In this retrospective case series, investigators from the University of Valencia, Spain, compared the three-year outcome of dental implants placed simultaneously or delayed with intraoral onlay block bone grafts before or at implant placement between 2005 and 2010. The parameters evaluated at follow-up visits were implant survival and success rates, peri-implant soft-tissue conditions (Plaque Index and Bleeding Index, probing depth, width of keratinized mucosa, and facial mucosal retraction), radiographic peri-implant marginal bone loss, and patient satisfaction. Thirty-four patients with 53 implants (23 delayed and 30 simultaneous) were included.
After three years of loading, the cumulative implant success rate was 83.3% for simultaneous and 96.9% for delayed implants (P = .217). Average marginal bone loss was 1.15 ± 1.67 mm for simultaneously inserted implants and 0.29 ± 0.35 mm for delayed implants (P < .01). There were no significant differences in Plaque Index or modified Bleeding Index between the groups. Peri-implant facial mucosal recession was more frequent in the simultaneous implant group (26.6% vs 13%), though the difference was not statistically significant. General patient satisfaction averaged 9.05 ± 0.82, and good quality of life was reported by all patients.
The authors concluded that despite its sample size and design limitations, the delayed procedure showed less marginal bone loss and a lower prevalence of facial mucosal recession than the simultaneous implant placement procedure at three years post-loading.
The areas I address above are important to all of us in our field. One of the many benefits of being an AO member is an automatic JOMI (bimonthly) subscription, which I read to stay up-to-date and be a better clinician. To learn more about becoming a member, visit osseo.org. You can also follow AO on Facebook, Twitter, and LinkedIn to stay current.