Why do prescription drugs cost so much in the United States?
Key Highlights
- Americans are cutting essentials like food and insurance to cope with rising health-care costs, highlighting the growing financial strain.
- While TrumpRx offers lower drug prices through a cash-pay model, it addresses symptoms—not the underlying causes of high pharmaceutical costs.
- A complex system of patents, regulations, and limited competition drives high prices, with true reform requiring fewer barriers and more market competition.
A recent survey revealed that Americans are cutting back on groceries and even dropping insurance just to survive health-care costs.
For Brown and others, those spiking costs are having real impacts on daily life. Of the 1,117 Americans surveyed who had ACA marketplace coverage in 2025, including those who dropped coverage or changed plans, about 55% said they’re planning to deal with health-care costs by cutting spending on food and other basic household needs.
So, when Washington suddenly rolls out a way to make certain drugs cheaper, people understandably cheer. That’s why TrumpRx—which gives people access to a growing list of prescription drugs at sharply lower cash-pay prices—is getting applause from both sides of the aisle.
On the surface, that sounds like a win. And for some people, it probably is. But it should also make you suspicious. Because if these drugs can suddenly be sold this much cheaper now, the question everyone should be asking themselves is: “Why were Americans being charged so much in the first place?”
The basic idea behind TrumpRx is pretty simple. It’s a cash-pay portal for dozens of prescription drugs. You still need a prescription, but instead of going through the usual insurance and pharmacy maze, you go through the portal and buy the drug directly at a posted cash price.
That price is based on a Most Favored Nation model. All that means is this: If a drug company is already willing to sell the same drug more cheaply in other developed countries, then Americans should get a similar low price too.
In other words, the government is saying: “If you can sell it for far less in Germany, Canada, or France … don’t turn around and charge Americans several times more.”
Also by the author: High fructose corn syrup and wasted taxpayer dollars
That’s the pitch. And again—I get why that’s attractive. If you’re paying absurd prices for insulin, semaglutide, or some other medication, you don’t really care whether the lower price came from a beautiful free-market process. You care that your monthly bill just got slashed. That’s why this kind of thing can get support from people across the political spectrum.
Even people who are usually hostile to Trump can look at cheaper drug prices and say: “Yeah, good. Finally.” But that still doesn’t answer the more important question: “Why were these drugs so outrageously expensive in the first place?”
Because that’s where the real problem is. You see, instead of curing the bureaucratic disease … TrumpRx just treats the symptoms. It may relieve some of the pain, but it does not remove the root cause of that pain.
The cycle that keeps Americans sick and poor
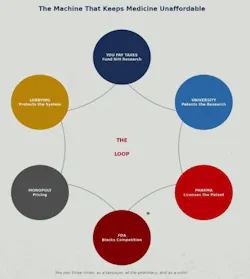
If you pull the curtain back, the story is not that complicated (figure 1).
- The government taxes you and funds research through agencies like the NIH.
- Then universities and research institutions turn those discoveries into patents and licenses.
- Then Big Pharma steps in with the legal protection and pricing power.
- Then the FDA piles on massive regulatory barriers that keep smaller competitors out.
The result is predictable: monopoly pricing, protected margins, and a lobbying machine that keeps the whole system in place.
That’s the loop. But whenever you point this out, people immediately say: “But pharma needs patent protection. They’re spending billions upfront to develop these drugs.”
That sounds reasonable until you look more closely. Yes, bringing a drug to market is expensive. But a lot of that expense is tied to the regulatory gauntlet itself—not just the natural cost of discovering and producing the drug.
One JAMA study found that for 59 new drugs approved in 2015–2016, the median direct cost of the key trials was just $19 million. Half of those drugs cost between $12 million and $33 million for those trials.
And those costs rose as trial demands rose—more patients, longer treatment durations, more complex endpoints. In other words, a lot of what gets called “development cost” is inseparable from the regulatory maze. And there’s another big problem with the “they paid for it all” story.
A huge share of the underlying science was funded by taxpayers in the first place.
A 2023 JAMA Health Forum study found that NIH funding contributed to 354 of 356 drugs (over 99%) approved from 2010 to 2019—totaling $187 billion in public funding. The authors concluded that, on comparable accounting, NIH investment was at least equal to industry investment. In short, the public helps fund the science, and then gets charged monopoly prices on the back end in return.
And when competition finally does break through, prices collapse—which tells you a lot about what was holding them up in the first place. FDA analysis found that with four generic competitors, generic prices were about 79% lower than the brand price before generic entry. With six or more competitors, prices were more than 95% lower.
That’s why companies fight so hard to keep competition out.
The FTC says “pay-for-delay” deals—where brand-name drug companies pay generic competitors to delay launching cheaper alternatives—cost consumers and taxpayers $3.5 billion a year in higher drug costs. That is not a free market. That is a government-protected racket.
If you want the full breakdown of that loop—including the FDA, patents, lobbying, and the role of middlemen, I break it all down in this video.
So, what would a real free-market prescription for America’s drug market look like?
Simple. Tear down the legal barriers that protect incumbents.
Make it easier for competitors to enter. Stop using patents, FDA gatekeeping, and regulatory complexity to artificially restrict supply. Let more producers make more drugs and compete on price. That’s the actual cure—not another government-imposed regulatory workaround.
You can’t solve problems caused by overregulation with even more regulation. That’s like trying to untie a knot by pulling it tighter. And this pattern is not unique to health care.
You see it in housing. Local governments restrict supply with zoning, permitting, density limits, and endless building rules. Prices go up and affordability collapses. Then politicians blame landlords, developers, or investors—and respond with more intervention.
You see it in higher education. The government floods the system with subsidized loans. Tuition rises and students get buried in debt. Then politicians step in with debt relief, repayment gimmicks, and even more subsidies.
You see it in childcare. Governments layer on staffing mandates, licensing rules, facility requirements, and all sorts of compliance costs that make childcare harder and more expensive to provide. Families get squeezed—and the political answer is more subsidies. It’s all the same pattern.
First, the government distorts the market. Then the distortion creates pain. Then politicians show up with a second distortion and call it the solution.
TrumpRx is part of the same thing. Yes, it may help some people in the short term. But it’s a workaround, not a cure. The cure is true free-market competition. It’s fewer legal barriers, fewer protected incumbents, and fewer politically engineered bottlenecks.
In other words: The cure is more market—not more management.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
About the Author

Joe Brown
Joe Brown is the founder of Heresy Financial. He is an entrepreneur, investor, public speaker, and host of the popular YouTube channel Heresy Financial, where he has helped millions achieve financial success by sharing key knowledge and insights on how the financial system works.