Peri-implant disease: Using artificial intelligence to predict those at risk
A new proof-of-principle study discusses the development of a machine that uses learned algorithms, a form of artificial intelligence (AI), that can analyze a dental implant candidate’s risk of developing peri-implantitis as well as their likelihood of a successful regenerative outcome after peri-implantitis reconstructive surgery.1 Peri-implantitis is a site-specific infectious disease that causes inflammation in the gum tissue and bone that surround the dental implant, resulting in loss of attachment. Depending on the definition and tissue loss threshold used in research studies, prevalence of this peri-implant disease is estimated to be around 20%–35% of implants in function after two years.2
Although dental implants have high long-term survival rates, their success rates are much lower and dental implants are subject to both biological and mechanical breakdown over years in function.3 With the increasing demand for dental implant therapy, combined with an increase in the number of dentists offering dental implant treatment, a rise in both dental implants being placed and dental implants suffering from disease has occurred. A method of predicting those at risk for dental implant disease can be a possible way of disease prevention, case selection, and increased patient oversight for those susceptible to attachment breakdown.
Related articles
- Dental implants fail at a rate 10 times that of natural teeth in patients with treated chronic periodontitis: New study
- Predictable tissue repair around diseased dental implants: The missing step
What is the global dental implant and implant disease market size?
The global dental implants market size was estimated at $7.87 billion USD in 2020 and was projected to reach $8.54 billion USD in 2021. The continued annual growth rate (CAGR) of dental implant treatment is 8.78% and market size is expected to reach $14.19 billion USD by 2027.4 Unfortunately, the global peri-implantitis market size was valued at $0.71 billion USD in 2019 and is expected to reach $1.4 billion by 2027 with a similar 8.7% CAGR.5
Depending on patient systemic and local factors, including the extent of tissue loss around a dental implant, decision matrices have been published in the literature that advise treatment modalities such as nonsurgical, surgical, or removal of the diseased dental implant.6 In addition, surgical protocols have been described that discuss both resective and regenerative forms of treatment.7 Because of advances in laser-assisted implant detoxification and growth-factor-enhanced regenerative treatments, the CAGR for these surgical forms of diseased implant treatment is expected to grow at the highest rate by 2027. Currently, there is no way to assess which patients are at risk for developing peri-implant disease and how they will respond to peri-implant disease treatment.
Using AI to predict successful regenerative outcomes
A team led by the University of Michigan School of Dentistry developed a machine-learning algorithm, called FARDEEP (Fast and Robust Deconvolution of
Not surprisingly, patients who were at low risk for periodontal disease showed immune profiles that were better at controlling bacterial infections around dental implants. A surprising finding from this study, however, was that the immune cell types that were better at controlling microbial infections were more important in determining successful regenerative outcomes than those that were better at controlling wound healing and tissue repair.
According to Dr. Lei, one of the researchers in the study, “Much emphasis has been placed on the immune cell types that are more adept at wound healing and tissue repair; however, here we show that immune cell types that are central to microbial control are strongly correlated with superior clinical outcomes. Surgical management can reduce bacterial burdens across all patients; however, only the patients with more immune cell subtypes for bacterial control can suppress the recolonization of pathogenic bacteria and show better regenerative outcomes.”
Conclusion
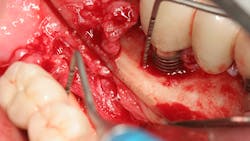
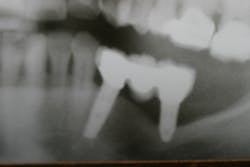
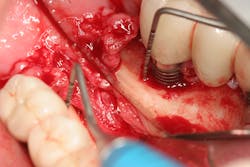
The expense and technical difficulty of removing an implant, rebuilding the defect, and replacing the failed dental implant with a new one can often be challenging. In addition, regenerative treatments for dental implant repair can be both costly and unpredictable if not done correctly (figures 1–3). Long-term maintenance and clinical oversight of peri-implant disease remains the most cost-effective and successful preventive measure for treating this disease.8 If this AI technology helps to determine the failure risk for the patient after surgical repair of the diseased dental implant, explantation with the replacement of a new implant or fixed/removable prosthesis may offer a better treatment alternative.
In the future, FARDEEP may be used to predict the risk of peri-implantitis before a dental implant is placed, but more trials are needed to explore this potential. For now, “this proof-of-concept study offers a personalized approach to identify the types of patients who better respond to regenerative therapies,” said coauthor Dr. William Giannobile, dean of the Harvard School of Dental Medicine.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Wang CW, Hao Y, Di Gianfilippo R, et al. Machine learning-assisted immune profiling stratifies peri-implantitis patients with unique microbial colonization and clinical outcomes. Theranostics. 2021;11(14):6703-6716. doi:10.7150/thno.57775
- Changi KK, Finkelstein J, Papapanou PN. Peri-implantitis prevalence, incidence rate, and risk factors: a study of electronic health records at a U.S. dental school. Clin Oral Implants Res. 2019;30(4):306-314. doi:10.1111/clr.13416
- Simonis P, Dufour T, Tenenbaum H. Long-term implant survival and success: a 10–16-year follow-up of non-submerged dental implants. Clin Oral Implants Res. 2010;21(7):772–777. doi:10.1111/j.1600-0501.2010.01912.x
- Dental implants market research 2022 – global forecase to 2027: increasing technological developments with rising product launches in the dental implants – researchandmarkets.com. Businesswire. https://www.businesswire.com/news/home/20220407005594/en/Dental-Implants-Market-Research-2022---Global-Forecast-to-2027-Increasing-Technological-Developments-with-Rising-Product-Launches-in-the-Dental-Implants---ResearchAndMarkets.com
- Peri-implantitis market size, share & trends analysis report by method type (surgical, non-surgical), by region (North America, Europe, APAC, Latin America, MEA), and segment forecasts, 2020 – 2027. Report ID: GVR-4-68039-099-7. Grand View Research. https://www.grandviewresearch.com/industry-analysis/peri-implantitis-market
- Tarnow DP, Chu SJ, Fletcher PD. Clinical decisions: determining when to save or remove an ailing implant. Compend Contin Educ Dent.2016;37(4):233-243.
- Froum SJ, Froum SH, Rosen PS. A regenerative approach to the successful treatment of peri-implantitis: a consecutive series of 170 implants in 100 Patients with 2- to 10-year follow-up. Int J Periodontics Restorative Dent. 2015;35(6):857-863. doi:11607/prd.2571
- Bernard S, Kotsailidi EA, Chochlidakis KM, Ercoli C, Tsigarida A. Implant and peri-implant tissue maintenance: protocols to prevent peri-implantitis. Curr Oral Health Rep.2020;7(3):249-261. doi:1007/s40496-020-00280-4
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.