Why do incision lines open, and what can I do about it?
When incision lines open and the graft and/or dental implants become exposed, it can be dramatic for both the dentist and the patient. Concerns regarding graft/dental implant infection, failure, pain, and poor healing ensue. The patient will often call the dentist in an emergency situation to ask for reassurance that “everything is normal.” This article briefly describes why sutures can fail and flap tissue opens, as well as options for treatment.
Dental implant contamination: 3 reasons behind a late-stage failure
Antibiotics: Are they needed for dental implant placement?
Why do stitches fail?
Suture failure with subsequent flap dehiscence and opening can be caused by a variety of factors:
- Social factors: smoking/vaping, alcohol use, hard foods, seeds, chewing on ice that disturbs clot formation and tissue maturation, positive pressure air flow (CPAP), asthma inhalers
- Poor-fitting prostheses: pressure from removable partial dentures, temporary flippers, overcontoured fixed bridges that press on flap tissue
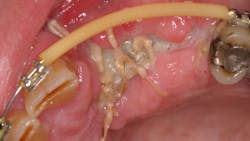
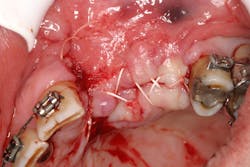
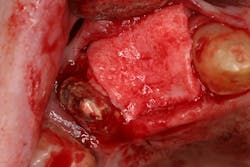
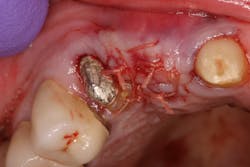
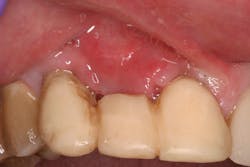
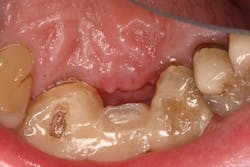
- Suture technique: lack of tension-free closure (figures 1 and 2), incision design doesn’t include keratinized tissue, failure to approximate tissue flaps (use of horizontal/vertical mattress helps)
- Surgical technique: failure to stabilize graft/membrane, lack of implant/cover-screw stability, insufficient amount of flap tissue in suture bite
- Systemic factors: diabetes, immunocompromised conditions, xerostomia, factors affecting blood flow, medications compromising blood flow/immunity
What are the treatments available when tissue flaps open?
In most instances if the incision lines open and the flap tissue dehisces, a watch-and-wait approach is advisable if the graft and issue are not infected. Typically, the exposed area will have junctional epithelium granulate in it and tissue coverage will occur. This usually takes a longer time and more oversight compared with areas of primary intention (flaps are approximated and closed).
Other treatments include:
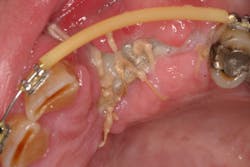
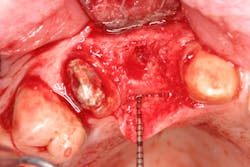
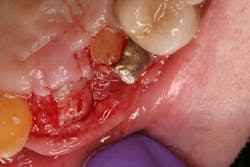
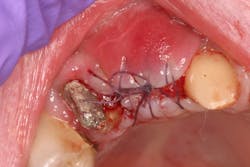
- Antiseptic mouthrinse. StellaLife has been shown to assist in tissue healing and prevent possible infections in areas of open wounds in multiple case series (figures 3–9).1
- Resuturing. This is potentially beneficial one to two days after surgery if the tissue flaps open. After that time, the tissue may be too friable to suture.
- Addition of biologics. Use of platelet-rich fibrin (PRF) and other growth factors that enhance angiogenesis have been shown to assist in wound closure.2
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Tatch W. 5 case series of accelerated healing after 5 different dental surgeries. StellaLife. December 21, 2022. https://stellalife.com/blogs/education/5-case-series-of-accelerated-healing-after-5-different-dental-surgeries-by-dr-walter-tatch-oral-maxillofacial-surgeon
- Naik B, Karunakar P, Jayadev M, Marshal VR. Role of platelet rich fibrin in wound healing: a critical review. J Conserv Dent. 2013;16(4):284-293. doi:10.4103/0972-0707.114344
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.