Options in anterior immediate implant placement
In the 1980s, we used to extract an anterior tooth, graft the socket, and delay implant placement to allow healing of the bone. This approach works well, but has two downsides: First, it extends treatment time and adds an additional surgery for the patient, and second, there can be unfavorable changes that occur in gingival form following the extraction and healing period.ALSO BY DR. FRANK SPEAR |Two fundamental etiologies of open embrasuresALSO BY DR. FRANK SPEAR |How to fix a deep overbite in wear patients There is a large quantity of research today that shows, in most instances, placing the implant immediately at the time of extraction is as successful as the delayed approach, it also eliminates one surgery, and reduces treatment time.
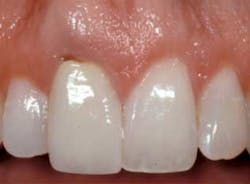
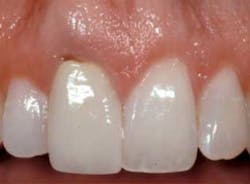
Immediate placement does have some challenges, however, and one of the biggest is managing the gingival form. Research shows that the greatest risk for an immediate single anterior implant is facial recession; the interproximal papilla is less of a problem as long as the adjacent teeth have normal bone levels on their interproximal surfaces. Because of this there are different approaches to immediate placement.Extraction, immediate placement with flap and grafting: This option is often used when there is a lack of facial bone on the tooth being extracted, and the surgeon desires the placement of a bone graft and membrane on the facial of the immediate implant. The use of this approach yields a predictable outcome with regard to the final osseous result, but typically leaves a flat gingival form that will require soft tissue augmentation at the time of uncovering the implant to get an ideal final result.Extraction, immediate placement without flap: There are multiple advantages to not laying a flap, the most significant being the option for managing the soft tissue at the time of implant placement. If the facial gingival margin on the tooth being extracted is at an ideal level, or coronal to ideal, it is possible to place the implant with a cover screw and then place a temporary which has an ideal emergence profile extending into the socket near the top of the cover screw. This temporary will help maintain the soft tissue form interproximally, and also on the facial, but won’t eliminate the risk of facial recession. There are multiple approaches to constructing the temporary on the day of surgery.Extraction, immediate placement without flap and immediate temporization: This approach is the most predictable from an esthetic soft tissue perspective. The tooth is extracted without a flap, the implant placed, and a temporary is placed directly on the implant at the time of surgery. This is only acceptable if the implant is well anchored in bone in the apical 1/3, typically requiring at least 35N of torque to reach final placement. This approach also allows the surgeon to place a facial connective tissue graft at the time of surgery to correct the facial gingival levels and thickness. The disadvantage of this approach is the time and necessity for the surgeon to fabricate the temporary. All the approaches above have been shown to be successful. Ultimately, the decision of which option to go forward with is mainly up to the surgeon and what he or she feels comfortable doing.Reprinted with permission from Spear Education.