Treating the geriatric dental patient
The older adult population in the United States is increasing dramatically with those over 65 expected to reach more than 89 million by 2050. Seniors over 85 are expected to reach 19 million during the same time frame. (1) The oral health report issued by the Surgeon General in 2000 contained a call for continued research among older Americans and the various oral health issues affecting them. (2) Because seniors are living longer, they are also keeping their natural teeth longer and will be increasingly seeking dental services. (3)
ADDITIONAL READING |Clinical care to comfort care ... a necessary continuum
Dental providers must be prepared to treat this population, requiring a thorough knowledge of geriatric issues, which are not just physical but social and psychological as well. Quality of life can be significantly affected by poor oral health. (4)
Many seniors are affected by one or more chronic diseases/conditions, which have various oral manifestations; and if the disease itself does not produce an oral manifestation, oftentimes the medication used to treat the disease will. (5) Most dental providers are aware that one of the most common chronic diseases of the elderly, diabetes, results in increased periodontal disease and delayed wound healing. Some may not be aware that enlarged salivary glands/xerostomia and oral candidiasisDental providers must also stay abreast of the many medications prescribed for senior adults treated in their practices, as they typically take several medications to control chronic conditions. The most common oral side effect of medications is xerostomia, which can lead to increased dental caries and periodontal issues. (6) Gingival recession is common among seniors subsequently resulting in an increased potential to develop root caries. The role of the hygienist in assisting the patient with plaque control is of utmost importance and can be quite challenging as many seniors experience decreased mobility and hand-eye coordination. They will need assistance in choosing products for maintaining optimum oral health, requiring different oral hygiene instruction than discussed with younger, more dexterous patients. An interproximal brush may be much more useful than dental floss, or a power toothbrush more effective than manual. Products for alleviating xerostomia may need to be prescribed such as xylitol or pilocarpine, and fluoride varnish may need to be applied to exposed root surfaces.
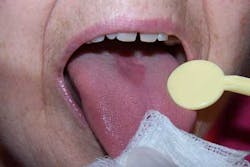
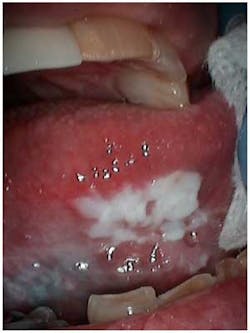
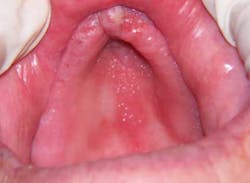
Oral cancer screenings are important for all patients, but even more so for the geriatric patient, as the majority of oral cancersAs our country experiences this dramatic increase in the older adult population, it would behoove the dental community to learn as much as possible about this complex population. The oral-systemic link has been well documented and will be even more important as we deliver comprehensive oral care to a large population of senior adults in the 21st century.
References
1. Vincent GK, Velkoff VA. The next four decades, the older population in the United States: 2010 to 2050. Current Population Reports: U.S. Department of Commerce, Economics and Statistics Administration, U.S. Census Bureau; May 2010. Report No.: P25-1138, Washington, D.C. http://www.census.gov/prod/2010pubs/p25-1138.pdf
2. U.S. Department of Health and Human Services. Oral Health in America: A Report of the SurgeonGeneral. Rockville, MD: US Department of Health and Human Services, National Institute of Dental and Craniofacial Research, National Institutes of Health, 2000.
3. Holtzman JM. Berkey DB, Mann J. Predicting utilization of dental services by the aged. J Public Health Dent. Spring 1990;50(3);164-171.
4. MacEntee MI. Quality of life as an indicator of oral health in older people. JADA. 2007;138;47S-52S.
5. Griffin SO, Jones JA, Brunson D, Griffin PM, Bailey WD. Burden of oral disease among older adults and implications for public health priorities. Am J Public Health. March 2012;102(3):411-418.
6. Turner MD, Ship JA. Dry mouth and its effects on the oral health of elderly people. JADA. 2007;138;15S-20S.
7. Silverman S. Mucosal lesions in older adults. JADA. 2007;138;41S-46S.
8. Vargas CM, Kramarow EA, Yellowitz JA. The Oral Health of Older Americans. Aging Trends; No.3. Hyattsville, Md.: National Center for Health Statistics, 2001.