Inflammation of the gingiva: The other reasons besides the obvious
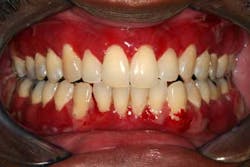
Gingival inflammation is usually attributed to bacterial-induced gingivitis and/or periodontitis. Although bleeding is most often caused by this etiology, there can be other systemic issues at work. The most common of these entities are the diseases listed under the category desquamative gingivitis. Desquamative gingivitis is a clinical term used to characterize attached and/or free (marginal) gingiva that demonstrates epithelial erythema and erosion. Desquamative gingivitis can be seen alone or with focal areas of ulceration. When a patient presents with desquamative gingivitis, the most common diseases or disorders that may be causing the problem are 1. (benign) mucous membrane pemphigoid, 2. erosive lichen planus, 3. lichenoid mucositis, and, less frequently, 4. pemphigus vulgaris. There are other diseases such as lupus erythematosus and erythema multiforme that under certain instances could be considered, but for our purposes we will address the most common entities.
OTHER ORAL PATHOLOGY ARTICLES ...
Diagnosis, causality, and risk factors
Vaginal Lichen Planus
Once you have clinically identified desquamative gingivitis, since all the causative entities can look clinically similar, the next step is to determine a definitive histologic diagnosis. This can be done with an incisional biopsy taken at the edge of a lesion so that the interface between normal and abnormal mucosa can be evaluated microscopically. The biopsy should be taken so that normal appearing tissue adjacent to the lesion is submitted along with the lesional tissue. If only ulcerated or eroded tissue from the center of an erosion or ulceration is submitted, there may not be enough diagnostic information to make a definitive diagnosis.
A conventional biopsy, placing the surgical specimen in 10% buffered formalin, is acceptable, but since two autoimmune diseases are in the differential diagnosis list, consideration should be given to direct immunofluorescence on the initial submission. Such specimens will need to be held in Michel’s solution instead of formalin for transport to the pathology laboratory. You can request Michel’s solution from the oral pathology laboratory you use. Michel’s solution has a relatively short shelf life compared to formalin, so contacting the lab a week or so prior to the biopsy procedure is all that is needed.
Once a definitive diagnosis is obtained, treatment for the diseases in the differential list will vary and are partially based on extent of involvement:
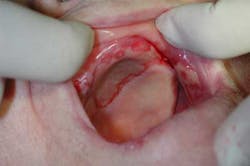
Pemphigus vulgaris (Fig. 1) can be a life-threatening disease and should be managed by either a vesicullo-bullous clinic or a dermatologist. Dentists can collaborate with their medical colleagues in treating the oral lesions, typically with an immunosuppressant (such as topical corticosteroids) or immune modulators (such as tacrolimus or dapsone).
Fig. 2
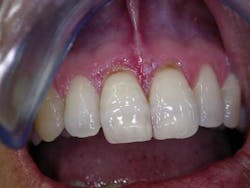
Lichen planus (Fig. 3) may also be treated in a similar fashion with topical corticosteroids, but patients with erosive lichen planus should be made aware of the reported increased risk of developing squamous cell carcinoma in involved areas. This risk is relatively small, but patients should be educated about it and reminded that their oral mucosa should be evaluated regularly. Initially, I see patients every three months. If they are disease-free, I may increase that up to a maximum of twice per year. In patients with a history of lichen planus or lichenoid mucositis, any ulceration that does not heal after two weeks of appropriate use of topical corticosteroid should be biopsied to rule out epithelial dysplasia or squamous cell carcinoma.
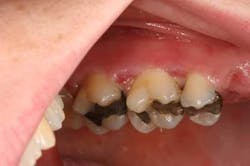
With lichenoid mucositis (Fig. 4), you and the patient need to become detectives to try to sleuth out the offending drug, supplement, product, etc., that might be causing desquamation and then have the patient discontinue the product. If a medication is found to be the etiology, consult with the patient’s physician to try to change the medication or the class of medication. If this is not possible, the patient will require palliative treatment for the periods of breakout, typically with a topical corticosteroid or immune modulator.