I'll have a maxillary anterior implant to go; please hold the periodontal treatment
Even though dental implants have historically enjoyed high survival and success rates (1), there has been a recent spike in the literature involving implant complications (2). Beginning in the last decade and continuing up until the present, it was quite common to receive solicitations for training seminars in dental implant placement and/or restoration. Recently, however, I have noticed that many more courses are geared toward identifying and treating implant complications rather than teaching routine implant dentistry. Unfortunately, this pendulum swing toward implant complication awareness is not unwarranted and is rooted in the fact that we are seeing an increase in the amount of implant-associated problems in our profession (3). A myriad of factors have contributed to this uptrend in implant complications, and many involve taking short steps in order to deliver an implant/implant restoration in a shorter period of time. In today’s financial-conscious economy combined with a digital technological era that can provide pretty much anything we desire with a swipe of the fingertip, the pressure to deliver a dental tooth replacement as soon as possible can drive a dentist to replace efficiency with expediency. This “fast-foodization” of implant treatment can often lead to complications and unforeseen repercussions as the time post implant crown delivery increases.
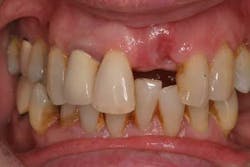
One prevalent shortcut that a practitioner can take is the failure to diagnose/treat periodontal disease prior to implant therapy. Because treatment of gingivitis and periodontitis can delay the placement of an implant fixture, both the practitioner and the patient may be tempted to avoid or postpone therapy until implant treatment is completed (Fig. 1).
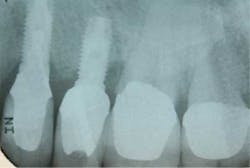
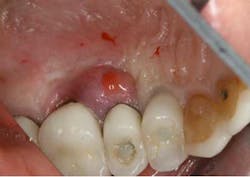
This financially expedient decision can have untoward consequences in terms of implant success. Numerous studies have shown that the composition of the microflora for both periodontitis and peri-implantitis is the same (4). In addition, other studies suggest that bacteria from a periodontally involved tooth can subgingivally colonize an implant placed in the same mouth within a two-week period of time (5). Overwhelming evidence suggests that periodontal therapy needs to be initiated prior to implant therapy in order to decrease the bacterial load that can infect dental implants and cause peri-implantitis. Other studies have shown that even in edentulous patients, periodontal pathogens can be located in reservoirs such as mucous membranes, saliva, and the pharynx. These bacteria can reinfect new dental implants placed in these patients, especially if they do not follow a proper hygiene and maintenance schedule (6). Because of these compounding variables, many studies suggest that there is an increase in biological complications associated with implants placed in patients who have untreated periodontal disease. In addition, patients with treated periodontal disease who received dental implants had a higher incidence of peri-implantitis when they were not on placed on a strict maintenance schedule when compared to those patients who were (7). For example, although the dental implant may not fail, the periodontally involved teeth next to an implant can develop problems and act as a conduit of bacteria to the adjacent implant (Figs. 2a and 2b). These bacteria can contaminate the dental implant and cause it to fail. In addition, common sense would also tell us that many of our patients have lost their teeth due to neglect and/or improper home care. Implants, although resistant to caries, are not immune to peri-implantitis or failure due to the same neglectful habits.
In summary, it behooves us as clinicians to deliver the best care possible to our patients. Unfortunately, this may mean delaying implant treatment in order to provide a better, safer foundation for our restoration. A healthier implant restoration can lead to a better long-term result compared to a quicker implant restoration.
Author bio
Scott Froum, DDS, is a periodontist and co-editor of Surgical-Restorative Resource e-newsletter. He is a clinical associate professor at the New York University Dental School in the Department of Periodontology and Implantology. He is in private practice in New York City. You may contact him through his website at www.drscottfroum.com.
References
1. Esposito, Hirsch, Lekholm, Thomsen. Biological factors contributing to failures of osseointegrated oral implants I. Success criteria and epidemiology. Eur J Oral Sci 1998; 106:521-557.
2. Lindhe J, Myle J. Peri-implant diseases: Consensus report of the Sixth European Workshop on Periodontology. J Clin Periodontology 2008; 35(suppl 8):282-285.
3. Karoussis IK, Müller S, Salvi GE, Heitz-mayfield LJ, Brägger U, Lang NP. Association between periodontal and peri-implant conditions: a 10-year prospective study. Clinical Oral Implants Research 2004; 15: 1–7.
4. Berglundh T, Lindhe J, Marinello CP, Ericsson I, Liljenberg B. Soft tissue reactions to de novo plaque formation at implants and teeth: An experimental study in the dog. Clin Oral Implants Res 1992; 2:1-8.
5. Quirynen M, Vogels R, Peeters W, van Steenberghe D, Naert I, Haffajee A. Clin Oral Implants Res. Feb. 2006; 17(1):25-37.
6. Greenstein, et al. Dental implants in the periodontal patient. Dental Clinics Of North America. Elsevier Ltd. 2010; 54(1)113-128.
7. Pjetursson, et al. Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care. Clin Oral Implants Res. Jul. 2012; 23(7):888-894.