Strategic retention of an ailing premolar with severe periodontitis using regenerative therapy: a case report
By Paul S. Rosen, DMD, MS There is a growing belief in dental practice today that if a tooth has advanced periodontal disease, it should be replaced with a dental implant rather than attempt to save it. Certainly, dental implants have been chronicled for their high level of success.1 But what if the loss of that tooth would lead to extensive restorative dentistry or the need for sophisticated procedures such as sinus elevation with concurrent bone grafting? Should the choice default to the implant or prosthetic option? Moreover, what about the patient’s desire to retain his or her own teeth? Regeneration is a treatment option for teeth with moderate to severe lesions that has demonstrated predictable success to achieve regeneration, new bone, cementum, and a functional periodontal ligament.2 Moreover, restoring these component tissues enhances the long-term survival of teeth.3 This case report documents one such instance where the loss of a premolar would have led to tremendous expenses for the patient for rehabilitation of this area.Case study This 63-year-old Caucasian female had been under routine periodontal maintenance care over the course of the last 10 years, having undergone comprehensive treatment that included surgery and rehabilitation with a fixed maxillary prosthesis. Her medical history was unremarkable except for osteopenia, for which calcium was taken. Maintenance visits were scheduled on a three-month interval and the patient was compliant with the prescribed care. Unfortunately, she experienced breakdown at the distal of the maxillary second premolar (Fig. 1) where clinical attachment loss and probing depths ranged up to 8 mm and mobility was 1+ degree. Furthermore, there was a separate but coincident periapical lesion (Fig. 2).
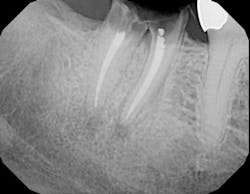
Fig. 1 — Pretreatment radiograph of the maxillary left second premolar. There is an advanced osseous lesion at the distal and suggestion of a developing periapical lesion.
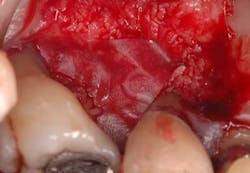
Fig. 2 — This view is taken after root planing. The lesion is a combined 1-2 wall that extends from the distal to the palate. What complicated care was that the tooth could not be extracted without incurring considerable costs. If the patient wished to replace this tooth with a fixed partial denture, she would need to have the existing seven-unit splint anterior to this tooth removed. If an implant was the desired option, the patient would need to undergo elevation of the sinus and — at the very least — wear a removable appliance until an implant could be placed and integrated, something she wished to avoid. The decision was to perform occlusal equilibration to eliminate fremitus in centric occlusion and excursive movements. Regenerative surgery was scheduled for this area that included elevation of full thickness flaps, meticulous debridement of the roots with hand and ultrasonic instruments, and root modification with tetracycline solution (Fig. 2). The root was then treated with a solution of a highly purified protein, recombinant platelet-derived growth factor (rh-PDGF-BB). The remaining/containing walls of the intrabony lesion were not ideal for space maintenance to stabilize a clot as their morphology had one to two wall components. To regenerate this site, an allograft of mineralized, freeze-dried bone (FDBA) (LifeNet Health, Virginia Beach, Va.) hydrated by rh-PDGF-BB was carefully placed into the defect to act as a biologic scaffold/clot stabilizer (Fig. 3). To further contain this graft-biologic composite, a barrier made from human chorion-amnion (BioXclude, Snoasis Medical Inc., Denver, Colo.) was placed over the graft-biologic and the flaps (Fig. 4) were secured with 6-0 expanded polytetrafluoroethylene (ePTFE) (W.L. Gore & Associates, Flagstaff, Ariz.), assuring complete closure of the site (Figs. 5 and 6).
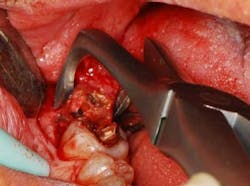
Fig. 3 — The composite graft has been placed after recombinant platelet-derived growth factor was applied to the root.
Fig. 4 — The barrier of amnion-chorion has been placed over the graft to facilitate its containment.
Fig. 5 — Buccal view of the suturing. Good primary closure has been achieved.
Fig. 6 — Palatal view of the area sutured. The sutures are composed of expanded polytetrafluoroethylene, which is monofilament to avoid bacterial wicking.
Postoperative infection control consisted of a systemic antibiotic — amoxicillin taken for the first seven days and the topical use of chlorhexidine mouth rinse applied to the site for the first month. For analgesia and the reduction of inflammation, ibuprofen 600 mg was prescribed for the first four to five days. The patient was seen approximately every 14 days for postoperative treatment during the three months. Sutures were removed at the first visit. She was then seen monthly up to the sixth postsurgical month. Postoperative visits included plaque debridement, polishing to remove stains, and oral hygiene reinforcement. The early frequency of visits was imperative as the patient had to refrain from both brushing and flossing of the treated area to provide wound quiescence until the clot had stabilized. After the first 30 days, mechanical oral hygiene was reinstated and the patient resumed her mechanical plaque control along with rinsing with an essential oil mouth rinse twice daily. Endodontics was completed at 28 days postsurgery to treat the apical lesion, and the patient resumed her typical three-month interval of maintenance care after the initial six months of stringent postoperative visits. The bone loss at the distal of this tooth has been substantially recaptured and the attachment level and probing depths have been restored to maintainable levels of 3 mm to 4 mm. Two years later, the bone levels have remained stable and the prognosis for this tooth has considerably improved (Figs. 7 and 8).
Postoperative infection control consisted of a systemic antibiotic — amoxicillin taken for the first seven days and the topical use of chlorhexidine mouth rinse applied to the site for the first month. For analgesia and the reduction of inflammation, ibuprofen 600 mg was prescribed for the first four to five days. The patient was seen approximately every 14 days for postoperative treatment during the three months. Sutures were removed at the first visit. She was then seen monthly up to the sixth postsurgical month. Postoperative visits included plaque debridement, polishing to remove stains, and oral hygiene reinforcement. The early frequency of visits was imperative as the patient had to refrain from both brushing and flossing of the treated area to provide wound quiescence until the clot had stabilized. After the first 30 days, mechanical oral hygiene was reinstated and the patient resumed her mechanical plaque control along with rinsing with an essential oil mouth rinse twice daily. Endodontics was completed at 28 days postsurgery to treat the apical lesion, and the patient resumed her typical three-month interval of maintenance care after the initial six months of stringent postoperative visits. The bone loss at the distal of this tooth has been substantially recaptured and the attachment level and probing depths have been restored to maintainable levels of 3 mm to 4 mm. Two years later, the bone levels have remained stable and the prognosis for this tooth has considerably improved (Figs. 7 and 8).
Fig. 7 — Image taken at two years’ post-treatment of the site, following a periodontal maintenance visit.
Fig. 8 — This two-year post-treatment radiograph demonstrates the favorable regenerative outcome that has remained stable. This is but one case example of the predictability of periodontal regeneration. The long-term outlook for this tooth is quite favorable, but only if periodontal maintenance is continued at three-month intervals. The benefits as mentioned are multifactorial, but most importantly, the patient’s desire to keep her tooth was achieved. Some might say that the added postoperative visits have been a burden. However, how many visits might have been involved had the decision been made to remove this tooth with the replacement being either an implant or a bridge? In conclusion, this course of selected care has been a cost- and time-effective means of achieving this patient’s ultimate desire to have a predictable method of care and to keep her tooth if it were reasonably possible.Author bio Paul S. Rosen, DMD, MS, maintains a full-time private practice in Yardley, Pa., limited to periodontics, surgical implant placement, and regenerative therapy. He is also a clinical associate professor of periodontics at the University of Maryland Dental School. Dr. Rosen is a diplomate of the American Board of Periodontology and serves as an examiner for the oral examination of the Board. Dr. Rosen has served on a number of committees for the American Academy of Periodontology. He is a reviewer for The International Journal of Oral & Maxillofacial Implants and serves on the Editorial Advisory Committees for the Journal of Periodontology, The International Journal of Periodontics & Restorative Dentistry, and The Compendium of Continuing Education in Dentistry. Dr. Rosen has authored/co-authored a number of articles on periodontal regeneration, implants, and interrelated orthodontic-periodontal care and revised the American Academy of Periodontology’s position paper on the “Treatment of Plaque-Induced Gingivitis, Chronic Periodontitis, and Other Clinical Conditions.” Dr. Rosen’s research helped develop and gain FDA approval for a novel approach to regeneration using a flowable polymer barrier. Dr. Rosen has lectured nationally and internationally on the subject of regeneration for both teeth and implants.References 1. Zarb GA, Schmitt A. The longitudinal clinical effectiveness of osseointegrated dental implants: the Toronto study. Part I: surgical results. J Prosthet Dent 1990; 63(4):451-457. 2. Bowers GM, Chadroff B, Carnevale R, et al. Histologic evidence of new attachment apparatus formation in humans. Part III. J Periodontol 1989; 60:683-693. 3. Cortellini P, Tonetti MS. Long-term survival following regenerative therapy of intrabony defects. J Periodontol 2004; 75(5):672-678.