The flipper dilemma: keeping patients out of the worst provisional option
I work pretty hard to keep patients out of flippers during implant therapy. They hate them with the fire of a thousand burning suns, and so do we. Patients don’t like that they’re removable and can be uncomfortable to wear. We don’t like them because there may be unintended soft tissue pressure, which can damage a healing graft or implant. But there’s another, more subtle reason to dislike these buggers: poor communication of esthetics.
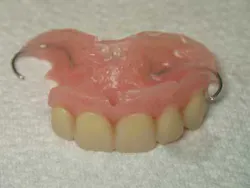
Fig. 1: An acrylic removable partial denture (flipper).
The following is a case study that shows how dentists can find creative solutions to the flipper dilemma.
Case study: creative solutions to the flipper dilemma
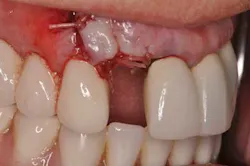
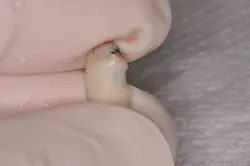
A patient presented with tooth No. 7 fractured to the level of the osseous crest. The tooth was deemed hopeless and treatment planned for extraction and immediate implant placement. (Figs. 2 and 3) Adjacent teeth Nos. 6 and 8 both had been restored with all-ceramic crowns. Ideally, a case like this would be immediately loaded, allowing (1) for the most accurate representation of the final esthetics during the healing phase and (2) a provisional restoration that does not rely on surrounding structures for support. Unfortunately, the patient was not a candidate for immediate loading and thus an alternative was required.Fig. 2: Immediately after implant placement, facial view.
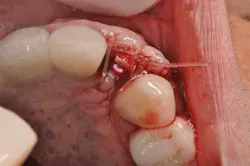
Fig. 3: Immediately after placement, occlusal view.
Rather than rely on an acrylic removable partial denture, the patient’s fractured tooth was used for the provisional restoration. It would be held in place with a fiber-reinforced ribbon that would be lightly bonded to the adjacent crowns. It was theorized that a Maryland bridge could potentially damage the adjacent crowns when ultimately removed. An Essix removable retainer was also considered, but the patient refused due to the added thickness to her remaining dentition.
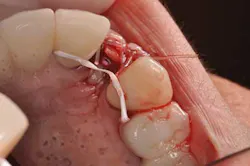
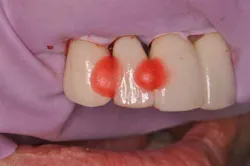
First, a piece of fiber-reinforced ribbon was cut and measured for fit to the adjacent teeth. (Fig. 4) Next, the patient’s fractured crown was modified in two ways. The intaglio area was filled with a composite resin and polished into the form of an ovate pontic. The crown then had a trough prepared on the lingual to house the ribbon material. (Fig. 5)Fig. 4: Measuring a piece of fiber-reinforced ribbon.
Fig. 5: Preparation of patient’s fractured tooth.A rubber dam was placed to protect the fresh surgical site from etching and bonding materials. The modified crown was held in the appropriate position while acrylic resin was applied on the facial. (Fig. 6) This was done to maintain the position of the crown while it was bonded from the lingual. Thirty-seven percent phosphoric acid-etch was applied to the lingual surfaces of crown Nos. 6, 7, and 8. Although 9.6% hydrofluoric acid etch can achieve a better bond to porcelain, the goal was only to achieve a temporary, lighter bond to the porcelain to reduce the chances of damage when the provisional would be removed. Bonding agent was applied and cured, followed by application of flowable composite. Flowable composite was also placed on untreated areas of interproximal porcelain for additional hold. (Fig. 7)
Fig. 6: Tooth held in place with acrylic resin.
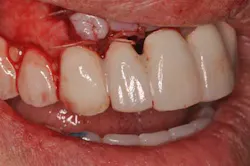
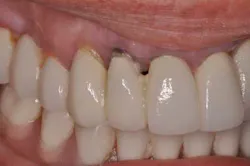
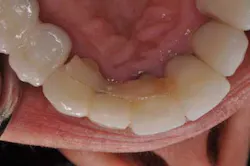
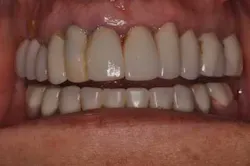
Fig. 7: Case immediately post-temporization.During osseointegration, the patient, restorative dentist, and surgeon were able to better visualize the soft-tissue dynamics and anticipate any potential problems. After four months of healing, the patient did not identify any cosmetic concerns save for the metal collar of the healing abutment being visible. (Fig. 8) The fiber-reinforced ribbon securely held the patient’s crown in place without complication. (Fig. 9) The next step of the provisional phase was to fabricate an implant-supported provisional restoration. This provisional allows for more detailed analysis of what will become the final soft-tissue esthetics of the case. (Fig. 10)
Fig. 8: Case after four months of healing, facial view.
Fig. 9: Case after four months of healing, buccal view.
Fig. 10: Implant-supported provisional to develop final esthetics.
ALSO BY DR. CHRIS SALIERNO ...
The wrong way to restore an implant
Long-term provisional success for young patients who need implants