How can you tell if a root is fractured?
Follow these five steps to determine whether a tooth root is fractured:
No. 1: Listen to the patient explain the history. They will tell you things like:
- “I used to chew on the tooth and get a sharp pain and then chew on the other side. Now the tooth hurts every time I chew.”
- “I used to avoid chewing on that tooth and now it hurts even when I’m not chewing.”
- “I used to avoid chewing on the tooth but now when I drink water or even breathe air, my tooth hurts.”
- “I had a root canal treatment done many years ago and everything was OK, but now the gum swells up around the tooth.”
- “I had a root canal done many years ago and everything has been fine, but now if I chew, the tooth hurts.”
- “My dentist told me I had a crack in the tooth and placed a crown. Now the tooth is painful.”
Tooth pain after root canal therapy: The 5 common causes
No. 2: Use a periodontal probe around the tooth.
Anesthetize the area with topical or local anesthetic, and then probe all six aspects of the tooth. Typically, you will find an isolated probing depth that occurs around a specific site near the fracture. Commonly this area is narrow and will be deep, especially if the fracture has alveolar bone involvement. A fracture can be especially likely with deep and narrow pocket depths when all other areas are within normal limits.
What is a periapical radiolucency?
No. 3: Evaluate the radiographs.
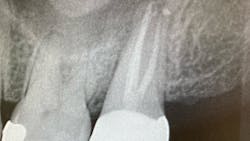
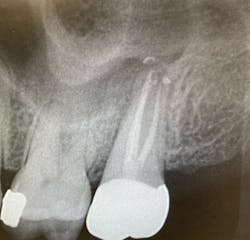
Check the radiograph for a lateral defect (lucency) in the bone with little or no apical disease (figure 1). Cases where the disease shows bone loss lateral to the root, but the previous root canal treatment looks to have been filled to the apex, are likely fractures.
No. 4: Evaluate a cone beam CT scan.
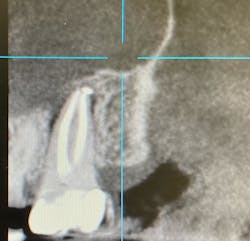
If you can use a CBCT scan, it will give you more detail and can be helpful in discerning the pattern of bone loss, although it won’t necessarily show the root fracture itself. Failure of endodontic treatment commonly occurs at the portal of exit apically (unless there is a lateral canal midroot). Fractures are typically present with lateral bone loss (figure 2).
No. 5: Look at the risk factors.
- Last tooth in the arch (especially lower molars)
- Few proximal contacts
- Presence of large post restorations
- History of fractured roots and crowns
- Parafunctional habits such as grinding, clenching, nail-biting, ice-chewing
- Lone-standing teeth (especially in the posterior regions)
- Poor crown-to-root ratio
- Endodontically treated teeth without cast restorations (especially molars)
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
About the Author
Omar Ikram, MRD, MClinDent, BDS, FRACDS
Omar Ikram, MRD, MClinDent, BDS, FRACDS, is an endodontist and practice owner of Specialist Endo Crows Nest based in Sydney, Australia's lower North Shore. He is also on staff at the Sydney Dental Hospital and is the president of the Australian Society of Endodontology—New South Wales Branch. Dr. Ikram completed his BDS in 1997 at Otago University and worked for approximately 10 years as a general dentist in New Zealand and England. His interest in endodontics led him to study a master's in clinical dentistry in endodontology at Kings College London, United Kingdom, followed by a Membership in Restorative Dentistry in the Royal College of Surgeons of Edinburgh. Contact him on Facebook and Instagram.