Introduction
Excessive gingival display (EGD) and “gummy smile” (GS) are descriptive terms, not diagnoses per se, but currently epitomize how clinicians and patients communicate on this topic. As patients are increasingly conscious of the role their smile plays in social and professional situations, they often self-refer for EGD correction.
Etiologies
Identifying any health problem’s source or etiology embodies the ideal goal of its therapy. For EGD, individual or combined etiologies can be dentoalveolar or nondentoalveolar in origin.
Dentoalveolar etiologies involve the teeth and periodontium, and include short clinical crowns, altered passive eruption (APE), gingival overgrowth, and/or dentoalveolar extrusion. Nondentoalveolar etiologies include skeletal and/or facial soft tissue anomalies, including hypermobility of the upper lip, short upper lip, and/or vertical maxillary excess (VME). We frequently identify APE and mild VME in GS cases in our periodontal practice.
Confirmation of VME by cephalometric analysis usually identifies a steep mandibular plane and an increased SN-GoGn angle (inclination of mandible relative to cranial base). This underscores the orthodontist’s role in identifying EGD, as it can become more apparent and recognizable after orthodontic treatment.
Because combined etiologies more commonly underlie EGD, multitreatment interdisciplinary approaches are frequently indicated. Biologic width (BW) is a fundamental concept that retains the clinician’s focus in periodontal-restorative discussions. BW is a zone of connective tissue and junctional epithelium between the alveolar crest and free gingival margin that must be preserved during restorative procedures to maintain periodontal homeostasis and avoid creating inflammatory processes in the dentogingival unit.
Preservation of both BW and the width of attached gingiva (even in unrestored anterior teeth) cannot be overemphasized in determining whether appropriate etiology-based EGD treatment(s) will include gingivectomy, osseous resection, or a combination of both.
Treatment of EGD
Most dentoalveolar causes of EGD can be effectively treated using restorative care, periodontal plastic surgical approaches, orthodontics, and/or surgically facilitated orthodontic therapy. Nondentoalveolar sources rely on orthognathic surgery (i.e., maxillary impactions), facial plastic surgical approaches, notably relying on myotomy or resection of the smile muscles through a nasal columellar incision. Botulinum toxin A effectively corrects GS for hypermobile lip and mild VME patients, but requires repeated treatment. A lip-repositioning procedure has been popularized recently to correct such GS cases permanently.
When APE is present alone or with other dentoalveolar factors, crown lengthening (CL) that includes gingival resection and/or osseous surgery can significantly reduce gingival display in full smile. Short or worn teeth may require restorations. Orthodontics may also be indicated to recover an extruded dentoalveolar complex.
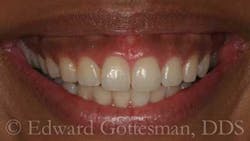
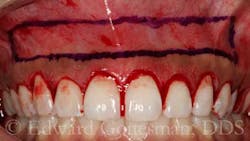
For VME, orthognathic surgery may be indicated. To mask mild to moderate cases of VME, and/or hypermobile upper lip, treatments such as reverse vestibuloplasty (i.e., lip repositioning) via a coronally advanced mucosal flap effectively shallow the vestibule, restricting mobility of the elevator smile muscles and upper lip. In the case of the 25-year-old Asian (Filipina) woman pictured in Figs. 1 through 8, the primary etiologies were APE, HUL, and VME.
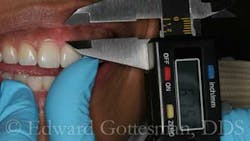
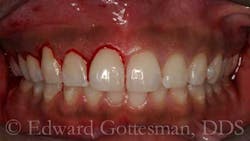
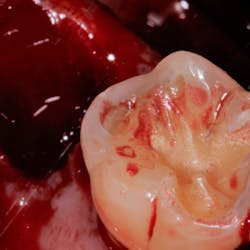
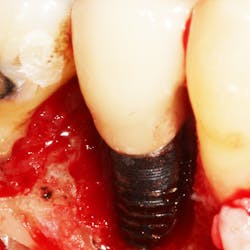
For this patient, CL via a gingivectomy only was necessary to expose the cementoenamel junction (CEJ) as the osseous crest is 2 mm to 3 mm apical to the facial CEJ (Figs. 3 and 4).
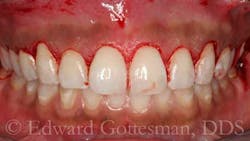
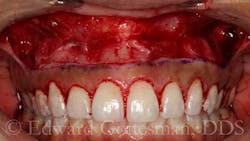
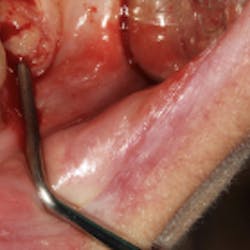
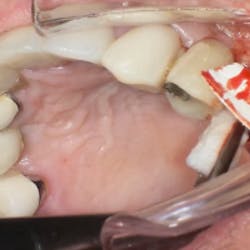
An elliptical incision removes a partial-thickness segment of vestibular mucosa and contiguous attached gingiva in a 2:1 ratio (Figs. 5 and 6).
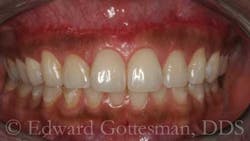
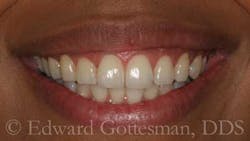
The apical margin of the mucosa is advanced coronally and sutured to the coronal margin of the attached gingiva, reestablishing the mucogingival junction at a more coronal level (Fig. 7), and effecting a pronounced reduction in gingival display during smile (Fig. 8).
When APE coexists with HUL and/or VME, combining this procedure with CL produces optimal results.
GS correction heralds significant esthetic dentistry milestones, allowing restorative dentists, periodontists, orthodontists, and oral surgeons to collaborate optimally in improving gummy smiles and changing people’s lives for the better.
Author bio
Dr. Edward Gottesman is a diplomate of the American Board of Periodontology and a fellow of the International Congress of Oral Implantologists. He received his DDS degree and completed his periodontal residency training at Stony Brook University School of Dental Medicine, State University of New York, Stony Brook, N.Y., where he is a clinical assistant professor. Dr. Gottesman is a partner at PerioNYC, a private periodontal and dental implant practice in Manhattan. You may contact Dr. Gottesman by email at [email protected] or visit www.perionyc.com for more information.