10 steps to perform an oral cancer screening
Squamous cell carcinoma (similar to skin cancer) of the oral cavity and throat account for about 45,000 cases each year in the United States, resulting in approximately 8,000 deaths per year.1 Studies show that successful treatment of oral cancer is highly dependent upon diagnosing and treating this disease in its early stages. Although there have been advances in surgical, chemotherapy, and radiation treatment for oral cancer, five-year survival rates of patients with this moderate to advanced disease are less than 60%.2 In addition, those patients who do survive typically have trouble chewing, speaking, eating, and smiling after treatment. It is, therefore, extremely important to diagnose oral cancer before it becomes advanced, since treatment for early cancer is not as severe.
ALSO BY DR. SCOTT FROUM | Human papillomavirus and oral cancer
Seventy-five percent of all head and neck cancers begin in the mouth, 30% of oral cancers originate in the tongue, 17% in the lip, and 14% in the floor of the mouth.3 Most common regions of oral cancer involvement are the back of the throat, the sides of the tongue, and underneath the tongue. Historically, smoking and alcohol use are highly related to the development of oral cancer and would affect people over the age of 50. Typically three out of four cases of this type of oral cancer in this age group were attributed to alcohol and smoking; therefore, increased screening in this patient type is warranted.4 Unfortunately, because of the increase in the incidence of human papillomavirus (HPV-16/18), head and neck cancers have been increasing in men and women in their 20s and 30s. One very general trend is that tobacco/alcohol lesions tend to favor arising in the anterior tongue and mouth, while HPV positive lesions favor arising in the back of the mouth.
The best way to detect oral cancer early is to perform a screening at every dental visit. The following is a brief description of the top 10 areas to examine and inspect (paraphrased and reproduced with permission from the Oral Cancer Foundation):5
Extraoral examination
The face: The entire face should be examined. Look for asymmetry, masses, swelling, discoloration, or ulceration. Evaluate for pigmented (red, brown, black), raised, ulcerated, or firm areas of the skin, including the hair-bearing regions of the face and scalp. The facial bones, skeleton, and soft tissue should be palpated, particularly noting asymmetry or masses.
The eyes: Extraocular movements should be checked in each direction to test for cranial nerve involvement. Any swelling of the eye or periorbital area should be noted and can be a late sign of a tumor. Drainage from the lacrimal system (epiphora) may be a sign of an obstructing mass in the maxillary sinus, nose, or facial soft tissue.
The ears and nose: Nasal examination should include palpation of the external nose and paranasal region overlying the maxilla and maxillary sinus. Hearing should be tested by talking with the patient during the physical exam and assessing the integrity of the acoustic nerve. Carefully inspect the auricle, noting any pigmented, erythematous, or ulcerous lesions. Note that skin cancers often appear on the superior, sun-exposed portion of the auricle.
The neck: The patient should be positioned at the dentist eye level. Bimanually palpate the neck, comparing both sides simultaneously for signs of enlargement of lymph nodes. Examine the jugular chain first. With two deeply placed fingers, palpate along the course of the sternomastoid muscles, underneath the mandible, and down to the clavicle. Palpate the supraclavicular spaces on either side. Examine the parotid groups lying anterior and inferior to the ears, the submental, and finally the submaxillary chain. To palpate a mass in the submaxillary area, insert a gloved finger in the patient’s mouth and press structures against your other hand, positioned under the chin. Next, palpate along the course of the larynx for signs of immobility or enlargement. According to the Oral Cancer Foundation, a patient over the age of 40 who presents with a neck mass that is painless, the first differential diagnosis should be oral cancer, and this not being the site of the primary, require a reexamination of the interior of the mouth to ensure that primary locations are identified. Enlarged nodes that are painless are seldom the result of an infectious process.
The thyroid: First inspect the thyroid gland and then palpate, because the thyroid gland is often difficult to feel. Some clinicians prefer to palpate the thyroid while positioned behind their patients, but it is perfectly acceptable to examine the gland from the front as well. Attempt to palpate the entire gland, and note the characteristics of any nodules or masses. Having the patient swallow while your fingers are positioned adjacent to the gland will elevate the thyroid gland and may facilitate your examination. Note and record any tenderness. After the lobe has been palpated, and with the fingers still, ask the patient to swallow. The gland will move upward during swallowing and any abnormality will become more apparent. On swallowing, the inferior pole of the lobes is elevated and can be outlined. Inability to palpate the inferior pole may suggest substernal extension of the thyroid gland on that side. Examine each lobe in this manner.
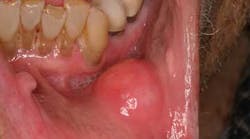
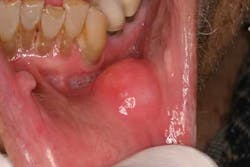
The lips: The lips should be evaluated with the mouth open and closed, noting any abnormalities in symmetry, contour, color, or texture. Attention to the vermilion border of the lower lip is warranted as this is a prime site for oral cancers. First, revert the lower lip and inspect the inner surface. The labial mucosa should be smooth and uniform in color. Notice the frenum of the lip in the midline. Note any signs of smokeless tobacco use (ulcers, red or white discolorations, texture variations) on the labial mucosa. With the lip still retracted, one can also inspect the gingivolabial sulcus, the gingival mucosa, and the teeth. Next, palpate the lip with your thumb and index finger, noting any firm or nodular submucosal areas (figure 1). Repeat these steps for the upper lip.
Figure 1
Intraoral cavity examination
Buccal mucosa: Move the buccal mucosa away from the teeth and gingiva to visualize the vestibule. Examine one side and then the other. It is not uncommon to see a white line (linea alba) from biting the cheek. Any irregularity in texture or color or other signs listed above should be noted. Be sure to examine the entire buccal mucosa from the labial commissure back to the anterior tonsillar pillar. Stenson’s duct from the parotid gland is a small protrusion in this area opposite the upper second molar and should secrete clear saliva from both sides when the parotid gland is milked. This area is easy to examine when two tongue blades are used to spread the lining from the gingiva or gauze is used to pull the lips apart. With your index and middle fingers inside the patient’s mouth on the buccal mucosa and with your thumb on the cheeks, carefully pull laterally and inspect along the upper and lower jaws. Next, gently pinch the cheek between your fingers and thumb; this allows you to palpate the buccal mucosa for any hidden masses.
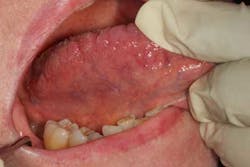
Tongue: Ask the patient to stick out his or her tongue and move it from side to side (figure 2). It should move easily and completely to both sides without spasm or asymmetry. Note any masses, ulceration, or swelling. When there is a nerve paralysis of the hypoglossal nerve, the tongue will usually deviate to the side of the lesion. Observe the dorsum of the tongue, noting any discolorations, irregularities, or limitations to movement, all of which may be a sign of cancer. Notice the circumvallate papillae and lingual tonsils, which are often mistaken for pathologic lesions. One of the most common sites of oral cancer is on the lateral border of the tongue, and it must be evaluated completely. This often requires using gauze to pull the tongue out and roll it from side to side while retracting the cheek with a tongue blade. A dental mirror may be necessary to visualize the base of the tongue (part of the oropharynx). This area is best viewed by pulling the tongue forward while holding it with 2X2 gauze, rolling it up into a position that enables a clearer view. Next, palpate the dorsum and lateral margins of the tongue, paying special attention to any masses or firm/fixated areas. Being careful not to gag the patient, palpate the lingual tonsils. Finally, have the patient touch the roof of the mouth with the tip of his or her tongue. This will allow the examiner to inspect the ventral surface of the tongue.
Floor of the mouth: The floor of the mouth is the U-shaped area that extends from the alveolar ridge of the mandible to the ventral aspect of the tongue. Inspect this area while the tongue is elevated. If needed, wrap a piece of gauze around the tip of the tongue and pull the tongue gently forward and to one side. With the other hand, use a tongue blade or gloved finger to push the middle of the tongue up and out of the way. Notice the frenulum in the midline and the ducts from the submandibular glands symmetrically on either side. Also note the sublingual glands. It is helpful to first dry this area with a gauze before looking for any surface abnormalities. Next, insert a gloved finger beneath the tongue, and another under the chin on the exterior skin, and bimanually palpate the submandibular glands and the entire submental region. Keep in mind that this one of the most common places for oral cancers.
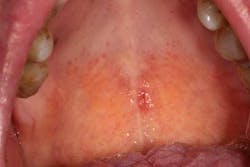
Figure 3
Hard and soft palate: Have the patient open wide and tilt his or her head backward to provide an adequate view of the hard and soft palate. If needed, depress the base of the tongue with a tongue blade to provide a better view of the soft palate. Loose teeth, red spots (figure 3), white spots, ulcerations, rough areas, asymmetry, growths, or other masses may be the first sign of a cancer in this area as in all areas of the head and neck. The uvula should hang down in the midline. Its deviation may indicate a vagal nerve palsy. Some patients have a torus palatinus, or bony outgrowth, from the midline of their hard palate. This variation of normal should not be mistaken for a malignancy.
Tonsils: Ask the patient to open wide, relax, and slowly breathe in and out saying, “Ahh.” This relaxes the tongue and offers a view of the oropharynx. It may be necessary to press down on the back of the tongue to get a full view of the oropharynx. Simply depressing the tongue with a tongue blade and having the patient say “ahh” often gives only a superficial view of the oropharynx, and many early cancers may go unnoticed. The palatine tonsils can be seen on both sides behind the retromolar trigone. Examine the anterior and posterior tonsillar pillars and tonsillar fossa for any exophytic mass, asymmetry, ulceration, or redness.
References
1. Ries LAG, Kosary CL, Hankey BF, et al. SEER Cancer Statistics Review. Bethesda, MD: NCI.2;1973-1995. American Cancer Society, Facts and Figures. 2000.
2. CDC MMWR: Preventing and Controlling Oral and Pharyngeal Cancer. US Department of Health and Human Services. August 28, 1998;(47).
3. National Cancer Institute. Surveillance, Epidemiology, and End Results Program public-use data. Rockville, MD: 1973-1998. National Cancer Institute, Division of Cancer Control and Population Sciences, Surveillance Research Program, Cancer Statistics Branch. Released April 2001, based on the August 2000 submission.
4. Silverman S. Demographics and occurrence of oral and pharyngeal cancers: The outcomes, the trends, the challenge. Journal of the American Dental Association. 2001;132(supplement):7s-11s.
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.