Gingival contouring using dental implant provisional restorations in the esthetic zone
Dr. V. Landon Blatter presents a case study to demonstrate how immediate nonocclusal load and occlusal load provisionals can be used to restore gingival contouring for dental implants placed in the challenging areas of congenitally missing maxillary lateral incisor sites.
Achieving appropriate gingival contouring in the smile zone is important in creating a pleasing smile. Congenitally missing maxillary lateral incisors typically have little gingival contouring present, so creating this gingival contouring can be challenging. The use of immediate nonocclusal load (INOL) or occlusal load (OL) provisional restorations can be helpful in these cases. This article discusses the use of INOL and OL provisionals to restore gingival contouring for dental implants placed in congenitally missing maxillary lateral incisor sites.
Immediate nonocclusal load provisionals
After a properly placed implant is inserted, a provisional restoration (utilizing INOL protocol) can be placed within 48 hours. (1) The use of INOL provisionals provides many benefits, including the following:
- Avoids a second-stage operation
- Retains gingival contours near the original position
- Offers immediate comfort and esthetics for the patient, as there is no need for a temporary removable prosthesis during the healing phase (2)
- Reduces the overall treatment time
Immediately loading a dental implant has many potential benefits; however, it might introduce micromotion and instability of the implant. (3–4) In turn, this micromotion may lead to implant failure. INOL provisional restorations should only have loading from the pressure of the lip and tongue and incidental contact with food, but not from occlusal forces of the opposing dentition. (1)
The predictable use of INOL provisionals requires that protocol be followed, and every implant system will have its own protocol for such provisionals. Generally accepted guidelines for INOL provisional restorations are as follows:
- 48 hours—An INOL provisional should be placed within the first 48 hours after implant placement. (1) Otherwise, the implant should be allowed to heal for three to six months (consult surgeon for preferable time frame) before placing a provisional. For more on this topic, read "5 questions to ask when determining if teeth with perio-endo infections can be saved."
- No occlusal stops on the INOL provisional from antagonistic teeth. This could lead to micromotion of the implant and possible implant failure.
- No excursive interferences on the INOL provisional, including no crossover interferences. Any interference can lead to micromotion and possible failure of the implant.
- No chewing on the INOL provisional restoration for the duration of the healing period. Again, micromotion of the implant is the concern.
- Open interproximal contacts preferred. Some clinicians feel micromotion from the adjacent teeth can be transferred to the implant if interproximal contacts are present.
- Understand the gingival biotype and the thickness of the gingival tissues. In my experience, a thick biotype with plentiful gingival tissue is more predictably sculpted than thin biotype.
Occlusal load provisionals
Occlusal load (OL) provisional restorations are utilized after the implant is integrated. It is appropriate to follow the same protocol as the INOL provisionals. However, since the implant is already integrated, the concern for implant failure caused by micromotion is diminished. The provisional restoration is fabricated in a similar manner as the INOL provisional—either at the lab or chairside.
In both the INOL and OL provisionals, the gingival tissues can be sculpted using the principle of gingival pressure. If pressure from the provisional is placed on the gingival tissues, then the gingival tissues will reshape to a position where the pressure is less. We can use this principle to create the gingival zenith in the desired position for an esthetic smile. Using pressure from the provisional is a predictable method to create a taller clinical implant crown. Taking pressure away will allow tissue to fill in, and as a result shorten, the clinical implant crown.
The use of gingival pressure can also help fill interdental papillary voids. When two natural teeth are adjacent to each other, the tip of the papillae can fill up to 5 mm from the intercrestal bone. When an implant is adjacent to a natural tooth, the tip of the papillae can fill up to 4 mm from the intercrestal bone. When two implants are adjacent to each other, the tip of the papillae can fill up to 3 mm from the intercrestal bone. (5)
The following case was treated in my office using the principles discussed above.
Case study
An 18-year-old female presents for implant crowns post orthodontic treatment. Maxillary lateral incisors were congenitally missing. The treatment plan was to allow complete growth before placing implants. We chose to allow complete healing of the implants before provisionalization and gingival sculpting. Temporary teeth were bracketed to the patient's orthodontic wires before the braces were removed; no gingival contouring took place while in the orthodontic temporaries. Implants were allowed to heal for four months while braces were in place.
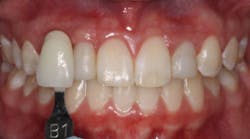
Immediately after removal of orthodontic appliances, gingival contours of the maxillary lateral incisors are not the appropriate height. See Figure 1. If left at this height, esthetics would have been compromised for this patient.
Figure 1
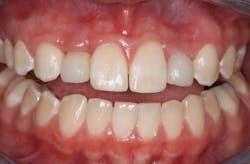
Provisional restorations were made from screw-retained temporary abutments with bis-acrylic temporary material mechanically locked onto the grooves of the temporary abutment. Figure 2 shows how the provisional restorations appeared immediately after chairside fabrication. Note that No. 10 has a better start to the gingival sculpting than No. 7. Also, note that the provisionals are short to be sure that they clear any occlusal contacts.
Figure 2
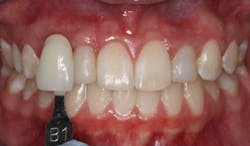
Figure 3 shows the provisional crowns after multiple reshaping visits. Note the gingival heights of No. 7 and No. 10 are much more esthetic than when the process began in Figure 2.
Figure 3
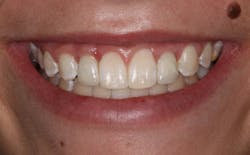
Final crowns are shown in Figure 4. The gingival contours of No. 7 and No. 10 are in a much more esthetic position—approximately .5 mm to 1 mm below an imaginary line connecting the zeniths of centrals to canines (6).
Figure 4
References
1. Laney WR, ed. Glossary of Oral and Maxillofacial Implants. Berlin, Germany: Quintessence Publishing Co Ltd; 2007.
2. den Hartog L, Raghoebar GM, Stellingsma K, Vissink A, Meijer HJ. Immediate non-occlusal loading of single implants in the aesthetic zone: a randomized clinical trial. J Clin Periodontol. 2011;38(2):186-194. doi: 10.1111/j.1600-051X.2010.01650.x.
3. Gapski R, Wang HL, Mascarenhas P, Lang NP. Critical review of immediate implant loading. Clin Oral Implants Res. 2003;14(5):515-527.
4. Trisi P, Perfetti G, Baldoni E, Berardi D, Colagiovanni M, Scogna G. Implant micromotion is related to peak insertion torque and bonedensity. Clin Oral Implants Res. 2009;20(5):467-471.
5. Tarnow DB, Eskow RN. Considerations for single-unit esthetic implant restorations. Compend Contin Educ Dent. 1995;16(8):778, 780, 782-784.
6. Contemporary concepts in smile design: diagnosis and treatment evaluation in comprehensive cosmetic dentistry. J Cosmetic Dent. 2014;29(4):132.