Dental implant contamination: 3 reasons behind a late-stage failure
Although dental implants enjoy a high survival rate in the clinical and academic literature, failures do occur.1 Implant failure can be divided into two types: early failure and late failure. Early failure occurs prior to the insertion of the abutment and crown complex, and late failure occurs after the dental implant has been loaded for a period of time.2 Late failure can be further subcategorized into mechanical and biologic complications. Mechanical complications usually involve damage to the prosthetic components or implant screw due to occlusal trauma and/or fatigue of the material. These complications can include fractures of the implant body, abutment, crown, supra-structure, and screw body.3 Biologic complications typically involve soft- and hard-tissue loss resulting from bacterial-induced disease.4
The literature suggests that the incidence of biologic complications over a 10-year period for a dental implant in function can be as high as 69%.5 In addition, many of these biologic complications involve dental implant contamination. Contamination can be prevented if the clinician can recognize the etiology, signs, and symptoms of these problems in their incipient stages.6 The aim of this article is to briefly describe three reasons for dental implant contamination.
Causes of dental implant contamination
No. 1—Contamination from an adjacent tooth
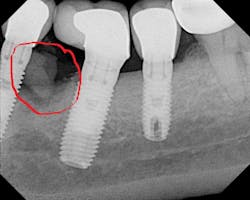
The literature is replete with case reports describing the infection and failure of a dental implant that is adjacent to a tooth with endodontic-induced apical pathology. Unfortunately, periapical lesions can travel to the dental implant and cause an exaggerated loss of attachment in a short period of time (figure 1).7 It is imperative that clinicians expeditiously diagnose and endodontically treat natural teeth with infections adjacent to dental implants.
No. 2—Contamination from implant cement
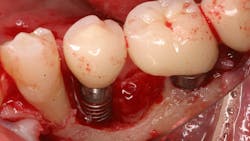
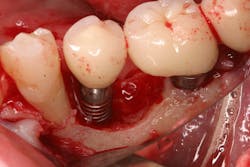
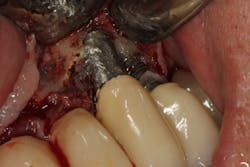
Once again, the literature is replete with case reports and case series describing soft- and hard-tissue loss due to excess dental cement left at the time of implant crown insertion.8 In one study, 90% of the implant crowns inserted with cement exhibiting inflammation and bleeding upon probing were due to cement in the peri-implant sulcus.9 Cement acts as a nidus for bacteria and induces a rapid hard-tissue loss around the dental implant fixture (figures 2 and 3).
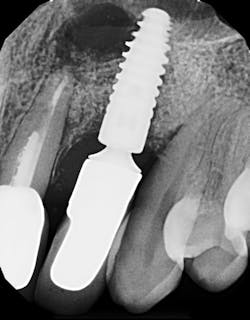
Detecting excess cement can usually be done with a radiograph if the cement is located in the interproximal region and is radiopaque (figure 4).
No. 3—Contamination from titanium particles
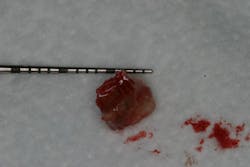
Recent studies have suggested that some biopsies taken of failing implants and their surrounding tissues contained titanium particles causing inflammation and tissue breakdown.10 These titanium particles are the result of implant surface sloughing either at time of insertion or over time, exposure to the oral environment, repeated instrumentation during hygiene, and/or instrumentation during implant disease debridement (figure 5).
Studies have shown that these breakdown particles can cause an inflammatory reaction that results in upregulation of osteoclasts.11 Because titanium particle-induced tissue breakdown is a relatively new topic, a dearth of information exists in the literature on treatment. One recent study suggests that during the debridement procedure of a diseased dental implant, a laser should be used to decontaminate the inside layer of the soft-tissue flap to ensure titanium particle removal.12
References
1. Pjetursson BE, Tan K, Lang NP, Brägger U, Egger M, Zwahlen M. A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clin Oral Implant Res. 2004;15(6):625-642. doi:10.1111/j.1600-0501.2004.01117.x.
2. Chung DM, Oh TJ, Lee J, Misch CE, Wang HL. Factors affecting late implant bone loss: a retrospective analysis. Int J Oral Maxillofac Implants. 2007;22(1):117-126.
3. Brägger U, Karoussis I, Persson R, Pjetursson B, Salvi G, Lang NP. Technical and biological complications/failures with single crowns and fixed partial dentures on implants: a 10‐year prospective cohort study. Clin Oral Implant Res. 2005;16(3):326-334. doi:10.1111/j.1600-0501.2005.01105.x.
4. Renvert S, Persson GR, Pirih FQ, Camargo PM. Peri‐implant health, peri‐implant mucositis, and peri‐implantitis: Case definitions and diagnostic considerations. J Clin Periodontol. 2018;45(suppl 20):S278-S285. doi:10.1111/jcpe.12956.
5. Stavropoulos A, Bertl K, Eren S, Gotfredsen K. Mechanical and biological complications after implantoplasty—A systematic review. Clin Oral Implants Res. 2019;30(9):833-848. doi:10.1111/clr.13499.
6. Klinge B, Klinge A, Bertl K, Stavropoulos A. Peri‐implant diseases. Eur J Oral Sci. 2018;126(suppl 1):88-94. doi:10.1111/eos.12529.
7. Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci. 1998;106(1):527-551. doi:10.1046/j.0909-8836..t01-2-.x.
8. Wilson TG Jr. The positive relationship between excess cement and peri‐implant disease: a prospective clinical endoscopic study. J Periodontol. 2009;80(9):1388-1392. doi:10.1902/jop.2009.090115.
9. Froum SJ, Froum SH, Rosen PS. A regenerative approach to the successful treatment of peri-implantitis: A consecutive series of 170 implants in 100 Patients with 2- to 10-year follow-up. Int J Periodontics Restorative Dent. 2015;35(6):857-863. doi:10.11607/prd.2571.
10. Mombelli A, Hashim D, Cionca N. What is the impact of titanium particles and biocorrosion on implant survival and complications? A critical review. Clin Oral Implants Res. 2018;29(suppl 18):37-53. doi:10.1111/clr.13305.
11. Trindade R, Albrektsson T, Tengvall P, Wennerberg A. Foreign body reaction to biomaterials: on mechanisms for buildup and breakdown of osseointegration. Clin Implant Dent Relat Res. 2016;18(1):192-203. doi:10.1111/cid.12274.
12. Rosen P, Froum SH, Froum S. A Rationale for post-surgical laser use to effectively treat dental implants affected by peri-implantitis: 2 case reports. Int J Periodontics Restorative Dent. In press.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and dental hygienists for issues relating to periodontal and implant medicine. Exclusive content from an academic perspective centers on complex care, solving clinical complications from a team-based approach through interdisciplinary management.
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.