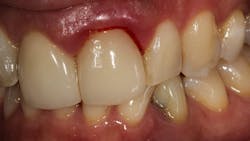
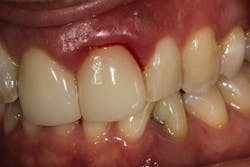
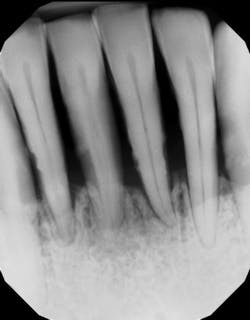
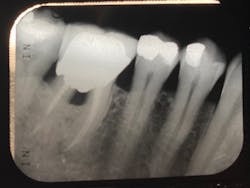
Gum bleeding after a dental cleaning
Recently several patients inquired about “why my gums still bleed” after they receive a professional cleaning with their dentists. The second question they ask is, “Is this normal?”
There are a multitude of reasons why patients may not respond properly to periodontal therapy or why their gums still bleed after a dental cleaning (figure 1).1 Of tantamount importance is to discern why previous therapy has not worked prior to reinitiating treatment or simply “giving the patient another cleaning.”
Studies have shown that multiple episodes of scaling and root planing (a deep cleaning) are no more effective than administering a single episode of scaling and root planing performed properly.1 The purpose of this article is to briefly discuss the top five reasons gingival inflammation persists after a dental cleaning.
No. 1: Residual calculus and bacteria remain after the dental cleaning.
There are several reasons why calculus and bacteria remain:
Pocket depth. Classic studies have shown that the deeper the periodontal pocket (the space between the gum and the tooth), the harder it is to remove the bacteria and calculus (tartar).2 For example, one study suggests that when probing depths are in the 1–3 mm range, removal of calculus during scaling and root planing can be 86% effective. That number drops to 32% when pockets are 6 mm or greater (figure 2).
antibiotic targeting, and/or periodontal surgery are necessary to identify the microbes and remove them.
No. 2: Operator experience
Traditionally, the more experienced the dental professional performing the treatment, the more effective the reduction of bleeding after a cleaning. One study showed that in moderate (4–6 mm) and deep (greater than 6 mm) periodontal pockets, operators with more experience produced a significantly greater number of calculus-free root surfaces after scaling and root planing than less experienced operators.7 The conclusion was that more experienced clinicians could be expected to render more effective root surface debridement.
No. 3: Patient home hygiene
Plaque, if left to accumulate after a dental cleaning, can cause the gums to bleed and may deepen the periodontal pockets. Suggestions for your patients:
- Proper brushing. Hold a soft toothbrush at a 45-degree angle and press it gently against the teeth where they meet the gum tissue. Move the brush back and forth, using short strokes, keeping the bristles in one place. Then move to the next section and repeat. Brush the outside and inside of all your teeth in the same way.
- Floss. At least once a day hold a piece of floss—12–18 inches in length—by wrapping it around your middle fingers and guide it between two teeth using either a thumb or index to pull against each tooth as you move the floss in an up and down direction. Another tool to use is the “floss pick” that has a small piece of floss preloaded on a plastic “fork.”
- Frequency. While you may decide to brush your teeth after every meal, full removal of plaque, as described above, needs to be done once a day.
No. 4: Medical history, genetics, and stress
Medical conditions that affect the immune system and bleeding disorders may cause patients to be more susceptible to bleeding of the gums before and after a dental cleaning. Genetics can also make an individual more susceptible to gum disease. When one is stressed or worried for long periods of time, the immune system will be weakened, making it harder for the body to fight off periodontal disease which may result in gum bleeding.
No. 5: Healing time after a dental cleaning
After a dental cleaning, patients may experience soreness and slight bleeding of the gums when brushing for a few days (24–48 hours), but after four weeks the bleeding should stop. If not, fractured calculus may be present under the gums. Explain to patients that they may need see a periodontist (a gum disease specialist) for more advanced periodontal treatment.
Conclusion
The importance of a staged treatment approach in periodontal treatment cannot be overemphasized. As with any wound, treatment begins with cleaning the wound as well as possible. That is what occurs in the initial cleaning or scaling and root planing visit. When that doesn’t work, bleeding and/or deepening of the periodontal pocket could result. The key is not to give up. It just means another diagnosis must be done, and treatment with more sophisticated instrumentation may be necessary to achieve the desired result.
All three authors have seen many patients throughout their careers who have been told that nothing can be done and that teeth need to be removed due to “uncontrollable periodontal disease.” In most cases, this has proven to be false. We have examined these patients and treated them with outstanding success.
If patients find that periodontal treatment is being repeated, gums are continuing to bleed, bad breath persists, and teeth are starting to loosen, they need to find a good periodontist—one who can help them achieve control of their periodontal disease and save their teeth.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Anderson GB, Palmer JA, Bye FL, Smith BA, Caffesse RG. Effectiveness of subgingival scaling and root planing: single versus multiple episodes of instrumentation. J Periodontol. 1996;67(4):367-373. doi:10.1902/jop.1996.67.4.367
- Rabbani GM, Ash MM Jr, Caffesse RG. The effectiveness of subgingival scaling and root planing in calculus removal. J Periodontol. 1981;52(3):119-123. doi:10.1902/jop.1981.52.3.119
- Chan HL, Oh TJ, Bashutski J, Fu JH, Wang HL. Cervical enamel projections in unusual locations: a case report and mini-review. J Periodontol. 2010;81(5):789-795. doi:10.1902/jop.2010.090654
- Cobb CM. Non-surgical pocket therapy: mechanical. Ann Periodontol. 1996;1(1):443-490. doi:10.1902/annals.1996.1.1.443
- Cobb CM, Sottosanti JS. A re-evaluation of scaling and root planing. J Periodontol. 2021;1-9. Published online: March 4, 2021. doi:10.1002/JPER.20-0839
- Xu W, Zhou W, Wang H, Liang S. Roles of Porphyromonas gingivalis and its virulence factors in periodontitis. Adv Protein Chem Struct Biol. 2020;120:45-84. doi:10.1016/bs.apcsb.2019.12.001
- Brayer WK, Mellonig JT, Dunlap RM, Marinak KW, Carson RE. Scaling and root planing effectiveness: the effect of root surface access and operator experience. J Periodontol. 1989;60(1):67-72. doi:10.1902/jop.1989.60.1.67
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.

John Sottosanti, DDS
John Sottosanti, DDS, received his undergraduate education at the University of Pennsylvania and his DDS degree from Georgetown University. His postdoctoral education in periodontics was at the University of Southern California (USC) School of Dentistry and the West Los Angeles VA Medical Center. For 27 years, he chaired and moderated the Annual USC Periodontal Symposium. Dr. Sottosanti has done original research on biofilm, calculus, and bone regeneration and has been a speaker at many regional, national, and international dental meetings. He is a past-president of the California Society of Periodontists and was elected to the American College of Dentists and the Pierre Fauchard honor dental society. Dr. Sottosanti has had a private practice in periodontics and implantology in San Diego, California, for many years.
Lee N. Sheldon, DMD
Lee N. Sheldon, DMD, is a periodontist in Melbourne, Florida. His practice includes two other dentists—Michel Furtado, BDS, a board-certified periodontist, and Matt Sheldon, DMD, a general dentist. Dr. Lee Sheldon and his office manager, Danyel Salmela, are founders of the American Association of Independent Periodontists, a mentoring group for periodontists seeking a more predictable way of practicing the business of periodontics in the current era. You may email Dr. Sheldon at [email protected].