To take the dental radiograph or not: that is the question
By Rebekah A. Duffy, RDHHow many times have you had a patient come into the office for a hygiene appointment and tell you, "I just went to the specialist/dentist and took so many X-rays, I don’t want to take anymore"?You are sitting in your operatory either running behind schedule or not wanting to run behind schedule, so you take the path of least resistance and say OK. Too often we let our patient’s wishes supersede what we know to be a correct treatment because, let’s face it, patient education takes time. In addition to our clinical measurements and assessments, dental radiographs provide us with a specific and accurate means of diagnosing disease and showing the patient problems that are evident. Even though our patients may have just received radiographs from the treating specialist or dentist, we cannot take for granted that an open margin, open contact, overcontoured restoration, residual cement, and/or a nonseated implant abutment was realized and treated (Figs. 1a through 1d). Not only do they allow us to discover iatrogenic dentistry, the benefits of radiographs also include the ability to ascertain interproximal caries, periodontal disease, abcesses or cysts, bony infections, and developmental abnormalities. The risks of not using the diagnostic capabilities of radiographs far outweigh the risk of radiation they possess.
Fig. 1a — Periapical radiograph taken three weeks after cementation of implant crown No. 20 during hygiene visit reveals excess cement on distal.
Fig. 1b — Periapical taken by hygienist reveals overcontoured No. 14 restoration that was resulting in a food trap and gingival inflammation.
Fig. 1c — Bitewing taken by hygienist three weeks after returning from an outside office reveals nonseated implant abutments on teeth Nos. 18 and 19. Patient complained of too many radiographs being taken.
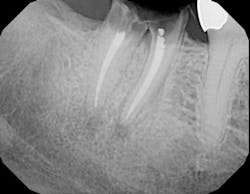
Fig. 1d — Radiograph taken by a hygienist in a specialty practice. Tooth No. 14 crown was inserted two weeks prior to visit without detection of recurrent decay on tooth No. 15.So what is that risk of radiation?According to the ADA1, the estimated exposure (in millisievert, mSv) is .038 for bitewing radiographs and .150 for a full-mouth series. The average radiation from a cone beam CT scan is .1 to .13 mSv. To give you a comparison, the added dose from cosmic rays during a coast-to-coast round trip flight in a commercial airplane is about 0.03 mSv, whereas radiation from outer space in Denver, Colo., per year is .510 mSv. The average radiation in the United States from natural sources is 3.0 mSv per year. This is not to say that dental radiographs pose no threat. We certainly want to minimize exposure, especially in our high-risk patients such as preganant women, breast-feeding women, and children.How often should we take dental X-rays?This answer, of course, depends on the individual patient, specifically age and disease risk. According to the ADA2, an adult (over 18) with a high caries/periodontal disease progression risk would need radiographs every six to 18 months. On the other hand, an adult with low risk would require X-rays every two to three years. Similarly, a child (under 18) with a high caries risk would need X-rays every six to 12 months vs. a low-risk child every one to two years. In summation, as hygienists, we not only have to be nonsurgical periodontal therapists, but we also have to be educators. We need to take that extra time and recite these timetables and exposure risks to our patients so they can have a better understanding of the importance of the dental radiograph. We also have to make sure that if the patient has traveled to another office to receive care, we don’t rely on other practitioners or assistants to have correctly identified possible pathology. The buck has to stop with us. Author bioRebekah A. Duffy, RDH, has been a hygienist in private practice for more than 10 years. She has lectured and written articles involving peri-implant maintenance and soft-tissue considerations. She currently works in a periodontal practice in New York City, N.Y.References1. Adapted from Frederiksen NL. X-Rays: What is the Risk? Texas Dental Journal. 1995; 112(2):68-72.2. American Dental Association, U.S. Food & Drug Administration. The Selection of Patients For Dental Radiograph Examinations. Available on www.ada.org.