Periodontal regeneration: Back to the future
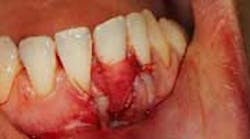
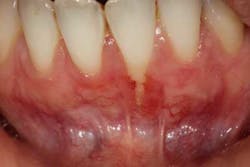
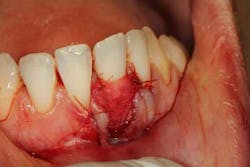
In 2014, the American Academy of Periodontology (AAP) held a workshop on periodontal regeneration to analyze the data on different methods of soft- and hard-tissue regeneration in order to rebuild the natural dentition both for esthetic and functional purposes. In 2015, the AAP took this body of research and published five different papers translating the findings into practical, take-home clinical applications that can be used in the office ("Practical Applications for Periodontal Regenerative Therapies—Clinical Advances in Periodontics"). Topics cover soft-tissue procedures for root coverage around areas of recession, as well as soft-tissue coverage to increase keratinized tissue in order to aid in oral hygiene. Evidenced-based advice is given on the best material to use in different situations based on both the local defects as well as considerations of the patient’s background—i.e., medical history, dental history, and social history.
Additional papers on both regenerating furcation defects and intrabony defects around teeth are presented that, again, present evidence-based decision matrices on which material is best to use in certain situations in addition to the predicted outcome of the procedure based on the challenge of the defect with the background of the patient. In subsequent articles, each of these topics will be presented and a summary of the seminal findings of these papers presented.
ALSO BY DR. SCOTT FROUM |Does your dental extraction socket need a bone graft: A decision matrix
One of the papers presented was on “Emerging Regenerative Approaches for Periodontal Reconstruction.” Since the 1960s, our field has been looking at new ways to grow bone and soft tissue around teeth. One of the major breakthroughs was when bone morphogenic protein, BMP, was isolated from human allograft. By combining our grafts with different regenerative growth factors and proteins, the field of dental science has been able to increase the success of our regenerative/reparative technologies and ultimately change the prognosis of hopeless teeth. “The availability of advanced diagnostic methods, the use of three-dimensional imaging modalities, the increasing access to optimized scaffold fabrication technology, and new surgical protocols and tools that minimize trauma and enhance wound healing are paving the road to a more predictable future in periodontal regenerative sciences.”
Specifically, this report mentions three new advances in regeneration. The first is the use of systemic anabolic agents in the form of teriparatide (parathyroid hormone). Self-administered by the patient into the thigh or abdomen, this 34-amino-acid molecule “acts on preosteoblasts to increase proliferation and also acts indirectly on osteoblasts to decrease osteoblast apoptosis.” Patients who received this treatment six weeks after open-flap debridement showed increased bone formation, especially in furcation regions one year after surgery.
ADDITIONAL READING |Guided tissue regeneration: background to current indications and applications
Another emerging approach to regeneration is the utilization of a controlled-release local delivery of rh-FGF. This growth factor, when combined with a cellulose carrier and delivered locally to the periodontal defect around the tooth, has shown significant improvements in percentage of bone fill compared with the cellulose carrier alone in Phase II clinical trials. Growth factors in general act to stimulate preosteoblastic cells upregulating differentiation into new bone as well as stimulating the inflammatory cascade, which promotes wound healing. Growth factor technology is commercially available today, such as platelet-derived growth factor, and has aided in increasing prognosis of natural dentition.
The final emerging technology mentioned in this paper is the use of stem cells. Stem cell applications have been studied for a long time in medicine and have a long history of debate. Their classification is divided into origin, embryonic stem cells, or somatic (adult) stem cells. Typical cells used in dental regenerative medicine are a type of somatic stem cell, the mesenchymal stem cell. Additional advances in dental stem cells have been the isolation of stem cells from both pulp tissue and PDL (this topic will be explored in another article). This paper discusses one commercially available product that has combined fresh frozen allograft with a vital mesenchymal stem cell component. This type of scaffold has shown promise in extremely challenging defects around teeth, again changing the prognosis of the tooth from one that would be extracted to something that can now be saved.