Does your dental extraction socket need a bone graft: A decision matrix
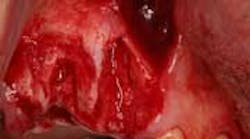
The dimensions of the residual edentulous alveolous after tooth extraction are critical to implant position and, therefore, the maintenance of the alveolar ridge after extraction is a crucial factor in determining the restorative outcome of implant placement. The normal postextraction healing response of an alveolar socket is resorptive. (1) Although unpredictable, the greater amount of alveolar ridge loss following extraction is usually horizontal in dimension along the buccal aspect of the ridge. (2) One highly quoted study suggests that 50% of horizontal ridge loss can occur after tooth extraction with an average of up to 6.1 mm (Figure 1). Two-thirds of this loss of bone volume occurred within the first three months. (3) Loss of vertical ridge height can also occur and usually takes place along the buccal aspect of the ridge to a lesser degree than horizontal ridge loss. (4) Corresponding reductions in vertical ridge height, ranging from 2.5 mm to 4.5 mm, have been noted. (5) The combination of this resorptive pattern results in a ridge that has moved in a palatal/lingual direction and has atrophied.
ADDITIONAL READING |Interdisciplinary management of a complex maxillary implant restoration
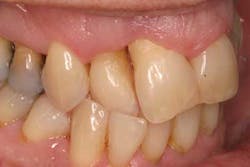
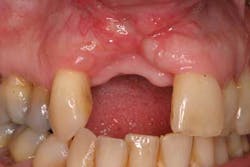
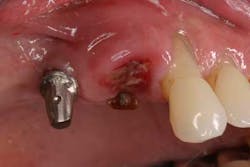
These alveolar bone changes often result in esthetic compromises in the area of tooth loss and can preclude ideal implant placement (Figures 2 and 2a). This situation is further exacerbated when the alveolus containing the tooth prior to extraction has lost bony walls or height due to periodontitis. In addition to the loss of hard tissue after tooth extraction, soft-tissue loss postextraction can also occur and result in a nonideal restoration. Surrounding soft tissues and interdental papillae are almost impossible to surgically re-create after being lost following tooth removal. (6)
Because of this alveolar resorptive pattern after extraction, the advent of grafting the extraction socket has become a solution that attempts to limit the amount of hard- and soft-tissue loss. Many studies have looked at the results of ridge dimension following tooth extraction after the use of an intrasocket graft with either an absorbable or nonabsorbable membrane, compared to extraction alone without grafting. Sockets that were preserved with graft and membrane on average lost 2.6 mm less ridge width and 1.2 mm less ridge height when compared to sockets that were not grafted. Maxillary sites lost more than mandibular sites, and most ridge resorption occurred on the buccal aspect of the ridge. (7)
With that in mind, does every extraction socket need to be grafted? The answer is no. The typical modified protocol I use is based on A Simplified Socket Classification and Repair Technique. (8)
Classification when existing tooth is still present:
Type 1 socket—buccal plate present; soft-tissue present
Type 2 socket—buccal plate missing; soft-tissue present
Type 3 socket—buccal plate missing; soft-tissue missing
Protocol: This protocol has modifications from the original suggestions and takes into consideration the geographic location of the tooth, albeit anterior or posterior as well as biotype (thick vs. thin).
Type 1a. (Thick biotype, posterior tooth, and buccal plate is present): NO GRAFT
Type 1b. (Thick biotype, anterior tooth, and buccal plate present): Collagen dressing
Type 1c. (Thick biotype, anterior or posterior, and buccal plate present): Bone graft
Type 2 socket—bone graft +/- membrane
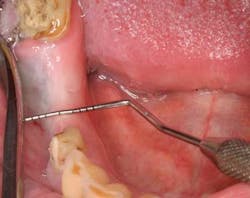
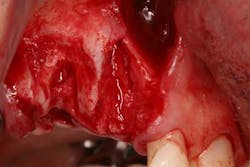
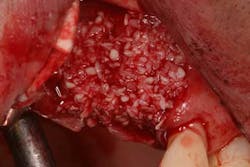
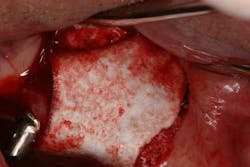
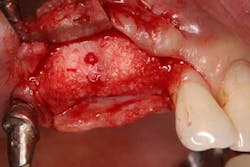
Type 3 socket—bone graft + membrane + biologic agent (if keratinized tissue is less than 2 mm, add a soft-tissue graft) (Figures 3, 3a, 3b)
ALSO BY DR. SCOTT FROUM …
Restoration of a damaged dental implant due to removal of a fractured screw: thinking outside the box
Diagnosing between ailing and failing implants: The haste to remove salvageable implants
References
1. Devlin H, Ferguson MJ. Alveolar ridge resorption and mandibular atrophy. A review of the role of local and systemic factors. British Dental Journal 1991;170:101-104.
2. Lekovic V, Kenney EB, Weinlaender M, et al. A bone regenerative approach to alveolar ridge maintenence following tooth extraction. Report of 10 cases. J Perio 1997;68:563-570.
3. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single tooth extraction: A clinical and radiographic 12-month prospective study. IJPRD 2003; 23:313-323.
4 Lekovic V, Camargo PM, Klokkevold PR, et al. Preservation of alveolar bone in extraction sockets using bioabsorbable membranes. J Perio 1998;69:1044-1049.
5. Lam RV. Contour changes of the alveolar processes following extraction. J Pros Dent 1960;10:25-32.
6. Park KB. Current soft tissue management in implant dentistry. IJPRD 1998;21:211-219.
7. Zubillaga G, Von Hagen S, Simon BI, Deasy MJ. Changes in alveolar bone height and width following post-extraction ridge augmentation using a fixed bioabsorbable membrane and demineralized freeze-dried bone osteoinductive graft. J Perio 2003;74:965-975.
8. Elian, et al.
About the Author

Scott Froum, DDS
Editorial Director
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of both the American Academy of Periodontology and the American Academy of Osseointegration, is in the fellowship program at the American Academy of Anti-aging Medicine, and is a volunteer professor in the postgraduate periodontal program at SUNY Stony Brook School of Dental Medicine. He is a trained naturopath and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him through his website at drscottfroum.com or (212) 751-8530.