Deciding between pink porcelain versus ridge augmentation in the esthetic zone
Although dental implants are a predictable treatment modality for the replacement of failed or lost teeth, the challenge continues to be achieving desirable esthetic outcomes in the maxillary anterior region that are acceptable to both patient and clinician. Hopeless teeth that warrant extraction in the maxillary esthetic zone due to severe caries and/or periodontal bone loss can often require grafting procedures to maintain bony volume. Adequate soft and hard tissue are necessary to restore esthetic dental implant contours.
Many times, however, this tissue is lost due to inadequate preservation at the time of extraction and/or tissue dehiscence and fenestration that yield volume defects. Once tissue is lost, the clinician is left with the decision to engage in tissue ridge augmentation prior to, during, or post implant therapy versus restoring the area with tooth-colored/gingival ceramic. The following two cases highlight two different approaches to reconstructing tissue defects during dental implant therapy, and considerations as to why that specific modality was selected.
ALSO BY DR. PETER MANN | A cost-effective method of creating a dental implant surgical guide for ridge augmentation
Case No. 1
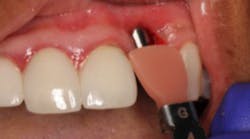
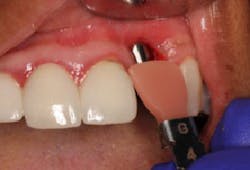
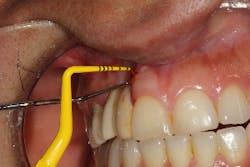
This patient presented with an unrestorable tooth No. 10 due to severe caries (figure 1). Prior to tooth extraction, the patient was informed that in order to avoid having a large defect, additional bone and soft-tissue grafting would be necessary. This type of augmentation would require additional time and finances, as well as increased surgical visits and appointments. The patient was informed that failure to undergo these procedures might result in (1) longer restorations, (2) the need for gingival ceramics, (3) inability to clean the prosthesis, and (4) increased forces on the implant because of the increased crown-to-implant ratio.
After considering her options, the patient chose not to have additional grafting. The reasons for her decision were her low smile line, a desire to keep case cost and time to a minimum, and her interest in function over esthetics.
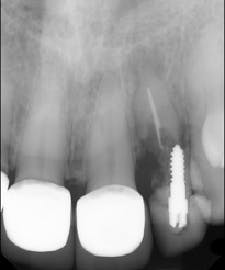
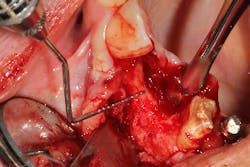
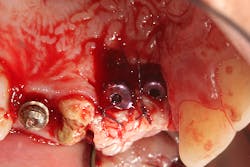
Tooth No. 10 was extracted. The socket was disinfected with chloramine-T gauze. An immediate implant (4.3 mm x 10 mm with a 5 mm healing screw) was placed (figure 2).
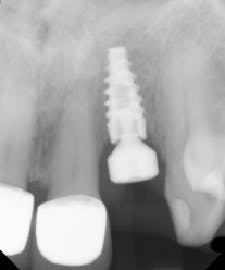
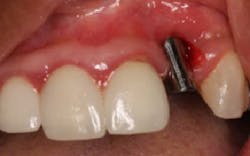
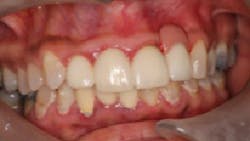
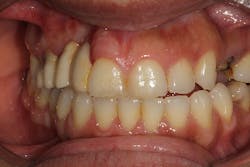
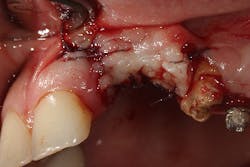
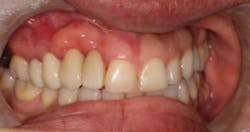
The patient presented to restore the implant six months later with a predicted large vertical and horizontal tissue defect (figure 3). The implant was restored with gingival ceramics to compensate for the ridge defect (figure 4).
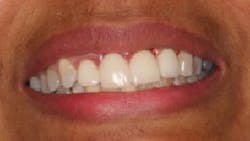
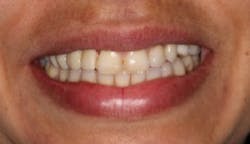
The patient was very pleased with the final outcome (figure 5), even though this case certainly would not be considered an esthetic success. Because of the patient’s concerns and low smile line (figure 6), this case was completed six months postextraction and in a cost-efficient manner.
Case No. 2
This patient presented with a long-standing edentulous area in the site of Nos. 6 and 7. She had lost both hard- and soft-tissue volume in the vertical and horizontal dimensions (figures 7 and 7a). Implant therapy was discussed as well as the option of multiple ridge augmentation procedures versus gingival ceramics. Although the patient has a low smile line, she was adamant about attempting to achieve a more proportional tooth length at final restoration. In addition, she complained about sensitive tissue underneath the pontic areas and an inability to clean her prosthesis. The periodontist and the patient decided to attempt to rebuild bony hard tissue and keratinized soft tissue. The patient understood the increase in finances and surgical procedures that would be involved.
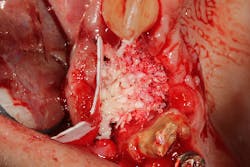
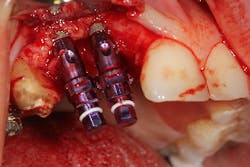
The patient was referred to a periodontist who first augmented the edentulous site with a hard-tissue graft and membrane (figures 8 and 8a). Six months later, implants were placed in ideal positon (figure 9).
At the time of Stage II, six months after implant placement, a palatal roll soft-tissue augmentation was performed (figures 10 and 10a). Six weeks later, the area was provisionalized with new temporaries to develop soft tissue.
Two years after the patient first presented with her edentulous site, the case was completed and the patient was extremely happy (figures 11 and 11a).
In conclusion, both patients were pleased with their outcome. In deciding which tool to use, managing patient expectations is crucial to a successful outcome. Communication with the patient and the specialist—in addition to setting a realistic outcome—will prepare the case for a pleasant conclusion.
ALSO BY DR. PETER MANN |Dental implants: The importance of patient compliance with immediate loading