Burning mouth syndrome: Etiology, symptoms, and treatment modalities
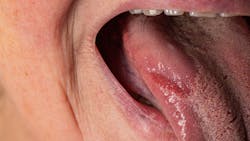
Burning mouth syndrome (BMS) is a chronic oral condition characterized by burning sensations and pain in the absence of clinical mucosal changes. It tends to affect more middle-aged and elderly women, typically on the tongue, lips, and hard and soft palate areas. Patients may also experience unremitting mucosal pain, dysgeusia, or xerostomia. BMS can be divided into two clinical forms: primary and secondary.
Types of BMS
Primary BMS is an idiopathic condition in which the cause cannot be determined; neuropathological causes are likely. Diagnosing primary BMS requires ruling out other etiological factors. Conversely, secondary BMS can arise due to local, systemic, and/or psychological causes; therefore, identifying its exact cause helps alleviate symptoms associated with BMS. When such factors are addressed or eliminated, treatment usually leads to significant clinical improvements in symptoms associated with this disorder.
You may also be interested in …
Poor diet decisions? Blame your genetics
Diseases most likely to affect the tongue and the importance of proper examination and diagnosis
Hormone levels and BMS
Recent research has demonstrated the role hormones can have in both the development and progression of BMS. Hormones—particularly those related to inflammation—have been connected with various symptoms, such as burning sensation, dry mouth, taste changes, and sensitivity to spicy foods. Studies have revealed that individuals with BMS tend to have higher levels of pro-inflammatory mediators like interleukin-6, -8, -10, and -12 than healthy individuals.1 Furthermore, these same cytokines were linked with higher salivary cortisol levels among patients with BMS.2
In addition to inflammatory markers, sex hormones appear to be involved in developing and treating BMS symptoms. Estrogen levels were significantly lower among postmenopausal women with BMS than non-BMS controls.3 Studies also suggest that reduced progesterone may contribute to BMS symptoms among both those who are postmenopausal as well as those on hormone therapy.
Some researchers have proposed a possible connection between thyroid hormones and BMS. They suggest that altered thyroid functioning could contribute to neuropathy or other issues leading to the development of BMS4; however, further investigation is necessary before any definitive conclusions can be made about this potential association.5
Nutritional levels and BMS
Assessing nutritional status when diagnosing patients with BMS is critical due to its potential effects on hormonal balance. Low nutrition can lead to anemia, which has been associated with lower production of hormones such as estrogen and testosterone that could exacerbate symptoms associated with BMS. Furthermore, certain vitamins and minerals are necessary for proper hormone balance, which helps mitigate some symptoms associated with the condition. Several therapies—vitamin replacement, zinc replacement, and hormone replacement—have been found to be effective in relieving oral burning or pain symptoms associated with BMS in those deficient in that factor.
Conclusion
Hormones and nutritional status can play a significant role in the development and progression of BMS. With proper assessment and treatment tailored toward modulating specific hormone and vitamin levels as well as necessary dietary modifications, patients may experience improved symptom management from this debilitating condition over time.
After eliminating potential causes, drug therapy should be initiated. Recent randomized, controlled clinical trials have suggested that drug therapy with capsaicin, alpha-lipoic acid, gabapentin, clonazepam, and antidepressants may provide relief of oral burning or pain symptoms.6 Psychotherapy and behavioral feedback may help eliminate BMS symptoms as well.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Barry A, O'Halloran KD, McKenna JP, McCreary C, Downer EJ. Plasma IL-8 signature correlates with pain and depressive symptomatology in patients with burning mouth syndrome: results from a pilot study. J Oral Pathol Med. 2018;47(2):158-165. doi:10.1111/jop.12666
- Gambardella A, Licata G, De Rosa A, et al. Burning mouth syndrome associated with tumor necrosis factor (TNF)-α inhibitor. Int J Dermatol. 2020;59(3):e70-e71. doi:10.1111/ijd.14681
- Nagamine T. Two-hit theory by estrogen in burning mouth syndrome. J Dent Sci. 2022;17(4):1833-1834. doi:10.1016/j.jds.2022.06.009
- Talattof Z, Dabbaghmanesh MH, Parvizi Y, Esnaashari N, Azad A. The association between burning mouth syndrome and level of thyroid hormones in Hashimotos thyroiditis in public hospitals in Shiraz, 2016. J Dent (Shiraz). 2019;20(1):42-47. doi:10.30476/DENTJODS.2019.44562
- Kumar K. Can thyroid cause burning mouth syndrome? MedicineNet. https://www.medicinenet.com/ can_thyroid_cause_ burning_mouth_syndrome/article.htm
- López-D'alessandro E, Escovich L. Combination of alpha lipoic acid and gabapentin, its efficacy in the treatment of burning mouth syndrome: a randomized, double-blind, placebo controlled trial. Med Oral Patol Oral Cir Bucal. 2011;16(5):e635-e640. doi:10.4317/medoral.16942
About the Author

Micaela Milano, MBA
Micaela Milano, MBA, is the owner and founder of Meraki Integrative, where she combines her extensive professional experience and passion for holistic health to deliver personalized, transformative care. Micaela holds an MBA in business, marketing, and management from Florida International University. In 2018, she founded the Meraki Initiative, dedicating herself to integrative wellness and client empowerment. A certified 200-hour yoga teacher, Reiki practitioner, and advanced holistic health coach, Micaela also holds certifications in angelic and crystal healing, bringing a deeply personal and spiritual dimension to her work. Her approach centers on addressing the root causes of health concerns, merging functional medicine with regenerative esthetics to support both inner vitality and outer radiance.