Improved dental implant surface and hygiene boost restoration success
Should a person’s teeth be saved at all costs? Over the last decade, the answer has shifted from yes to no in favor of replacing diseased and damaged teeth with implants. But treatment of patients with periodontitis, inflammatory disease of ligaments and bones supporting teeth, remains controversial because artificial tooth roots are more likely to fail.
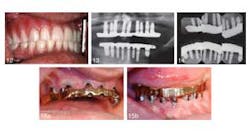
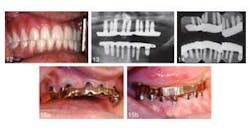
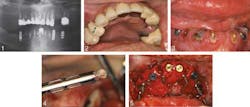
An article in the current issue of the Journal of Oral Implantology looks at long-term treatment for a patient with severe periodontal damage. The authors anticipate that the higher risk of implant failure in this patient will be offset by coating the implants with a rough, oxidized surface called TiUnite and by emphasizing the need for diligent oral hygiene. They also expect that by using overdenture prostheses instead of conventional removable dentures, they will improve stability and function — and thus patient satisfaction. Overall, increased use of implants has improved eating comfort and resulted in few complications after the surgery. However, pressure on implants is suspected to speed up loss of dense cortical bone in the jaw. Research has shown the TiUnite material stimulates bone growth, leading to faster fusion of implants and surrounding jawbone.RELATED | New material used in molar extraction sites optimizes bone regeneration and dental implant stability The current article is a case report on a 51-year-old patient who had been in a motorcycle accident and has a history of herpes, hepatitis, insulin-dependent diabetes, and persistent recurrent tooth decay. The patient’s remaining teeth (see photos below) were comprised of fractured crowns and older failing implants. The surgeons removed all of his teeth and old implants followed by the immediate insertions of new implants and stabilizing overdentures. Provisional implants were used for support during healing. Five months later, the interim provisional implants and prosthesis were removed and fabrication of a final restorative prosthesis was initiated.
RELATED | Atrophic patients have more options with new dental implant Despite the higher risk of implant failure due to his periodontal disease and diabetes, the patient’s implants have been in place for 12 years with no complications noted at routine checkups and cleanings. The patient has been instructed post surgery in proper use of floss threaders, deep-cleaning brushes, and an oral irrigator. His daily efforts to practice good oral hygiene improved his overall dental health. The patient was pleased with the results one week after the provisional implants were placed and was still happy with the surgery 12 years later. Little care and maintenance of the prostheses have been necessary.RELATED |Less invasive approach to dental implants allows heart patients to continue anticoagulation therapy
The authors concluded that in this case the prostheses have been effective, predictable, and reliable. They contend that such positive results were only possible because the patient changed their at home oral care preventing plaque buildup and disease. Full text of the article “Twelve-year clinical and radiological results of a maxillary and mandible implant-retained bar overdentures carried out on oxidized (TiUnite) replace select implants: A clinical case,” Journal of Oral Implantology, Vol. 39, No. 6, 2013, is now available here. The Journal of Oral Implantology is the official publication of the American Academy of Implant Dentistry. For more information about the journal or society, please visit their website.
The authors concluded that in this case the prostheses have been effective, predictable, and reliable. They contend that such positive results were only possible because the patient changed their at home oral care preventing plaque buildup and disease. Full text of the article “Twelve-year clinical and radiological results of a maxillary and mandible implant-retained bar overdentures carried out on oxidized (TiUnite) replace select implants: A clinical case,” Journal of Oral Implantology, Vol. 39, No. 6, 2013, is now available here. The Journal of Oral Implantology is the official publication of the American Academy of Implant Dentistry. For more information about the journal or society, please visit their website.