Dental hygiene nightmares no more: At-home maintenance for success with dental implants
The importance of plaque removal for the prevention of dental and systemic diseases has been well-documented in the literature. Dental hygiene maintenance programs tailored to the specific patient have become an important aspect of dental care, with approximately 50% of the adult population suffering from periodontal disease and the known increase in the prevalence of peri-implant disease. (1)
Disease progression from gingivitis to periodontitis around natural teeth is very similar to the progression of peri-implant disease from peri-implant mucositis to peri-implantitis, since the etiologic pathogenic bacteria are the same. (2,3) In addition, studies show a similar inflammatory cascade initiated during the disease process of both teeth and dental implants. Similar to periodontitis, peri-implant disease is multifactorial and influenced greatly by individual patient factors. (4) One of the biggest determinants of disease progression is adherence to a proper home-care dental hygiene regimen. (3)
READ MORE |Antibiotic resistance and periodontitis
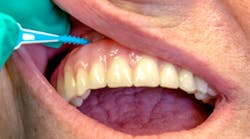
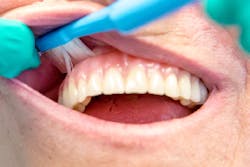
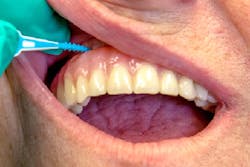
Understanding the products that patients can use to clean natural teeth and maintain dental implants is imperative if you are to provide appropriate advice about the challenging task of at home maintenance. Interdental brushes serve as an alternative to flossing, can be used daily, and—as suggested by a number of studies—can be more effective for interproximal plaque removal than floss. Interdental brushes with plastic-coated wires, depending on their size and shape, can be effective tools for reducing interproximal plaque (figure 1). (5) Other considerations for recommending interdental brushes include an individual's manual dexterity, how easy the product is to use, and the patient’s motivational level.
Taking time to sit with your patients and find the best hygiene tool(s) for their specific appliance and capabilities are crucial. Moreover, the benefits of plaque reduction around teeth and implants can improve oral and overall systemic health. We can no longer accept a one-tool-for-all approach; at-home maintenance routines need to be customized.
References
1. Kielbassa AM, Muller J, Gernhardt CR. Closing the gap between oral hygiene and minimally invasive dentistry: a review on the resin infiltration technique of incipient (proximal) enamel lesions. Quintessence Int. 2009;40(8):663-681.
2. Jepsen S, Berglundh T, Genco R, et al. Primary prevention of peri‐implantitis: managing peri‐implant mucositis. J Clin Periodontol. 2015;42(S16):S152-S157. doi: 10.1111/jcpe.12369.
3. Tarnow D. Increasing prevalence of peri-implantitis: how will we manage? J Dent Res. 2016;95(1):7-8. doi: 10.1177/0022034515616557.
4. Marcantonio C, Nicoli LG, Marcantonio JE, Zandim-Barcelos DL. Prevalence and possible risk factors of peri-implantitis: a concept review. J Contemp Dent Pract. 2015:16(9):750-757.
5. Schmage P, Platzer U, Nergiz I. Comparison between manual and mechanical methods of interproximal hygiene. Quintessence Int. 1999;30(8):535-539.
6. Wingrove SS. Peri-implant therapy for the dental hygienist: clinical guide to maintenance and disease complications. Hoboken, NJ: Wiley-Blackwell; 2013.
7. van Velzen FJ, Lang NP, Schulten EA, Ten Bruggenkate CM. Dental floss as a possible risk for the development of peri‐implant disease: an observational study of 10 cases. Clin Oral Implants Res. 2016;27(5):618-621. doi: 10.1111/clr.12650.