The dental interdisciplinary enhancement of cosmetic results via communication
Achieving a successful result in the maxillary anterior esthetic zone is often a challenge both from a technical standpoint as well as a communicative standpoint. A practitioner must have the knowledge, skill, and communication among his or her team members in order to maximize the potential for an outcome that will not only be suitable for the patient, but also encourage referrals. Assuming that the practitioner has the knowledge and the skill to endeavor into maxillary cosmetics, this article will focus on the communication that should occur among team members discussed in the format of a recent case result. In addition to my office, my team consists of the surgeon, the lab, and the patient.
ALSO BY DR. MICHAEL WEI |Smile makeovers without the expense
Communication with the patient
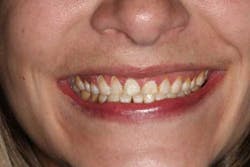
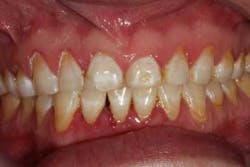
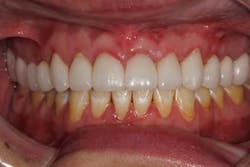
The start of a good doctor-patient relationship begins with an accurate history taking; in addition to establishing the patient’s chief complaint, a detailed medical, dental, and social history should be recorded. In this case, the patient was a 31-year-old female with a noncontributory present medical history, taking no medications, and having no known food or drug allergies. Her chief complaint was that “she was getting married and hated her smile.” She was conscientious of having “yellow, short, lifeless, and disproportional teeth that needed to be fixed before the wedding, so I can have a beautiful, gorgeous, white, bright smile.” She had a medical history consisting of bulimia for many years, which affected her dentition. After years of acid exposure and bruxism, her enamel had deteriorated, discolored, and become soft. She had lost vertical dimension and, more importantly, her confidence. (Figs. 1 and 1a) After all of the information was gathered, a realistic treatment plan was given to the patient: vertical dimension was to be opened to increase tooth length, crown lengthening was needed in order to even out gingival margins as well as increase tooth length, and all-ceramic crowns (e.max all-ceramic crowns) were to be placed from Nos. 2 through 15 because of both cosmetics and soft dentition. Once the treatment plan is accepted in theory, a financial conversation must take place (a topic for another article).
An extremely important note in this case was the patient’s refusal to be referred to a periodontist for crown lengthening at first, and an ultimatum given to the patient that I would not engage in this treatment without her having this procedure. The importance of crown lengthening to a successful outcome was emphasized to the patient and is incumbent upon us as general practitioners not to compromise our treatment or knowledge of biology by accepting compromise.
Communication with the laboratory
Communication with the laboratory is tantamount to success in most anterior esthetic cases. Most conversations take place between dentists and lab technicians only when there is a problem. The majority of problems between dentists and laboratories are due to the result of miscommunication. For example, the dentist will write on a lab script “please fabricate wax-up” and expect that the lab will know what the dentist wants. Although I work with NuLife Long Island, a very well-known and capable lab, I still will send in photos and models with a detailed lab script of what I am looking for. The lab script will include: midline relative to lip line, tooth symmetry, tooth axis, gingival margins and zeniths, morphology of the tooth based on age and sex of patient, incisal edge position and angle, interdental contacts, texture, and finally color. I also look at the patient’s facial features that will complement his or her overall smile. After the lab receives the script, a long, detailed conversation occurs either by phone or by email. Once I receive and approve the wax up, the patient needs to approve it prior to proceeding.
Communication with the specialist
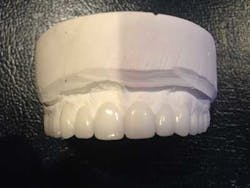
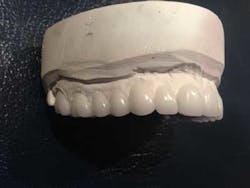
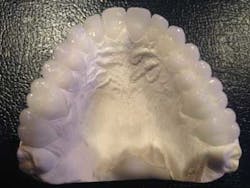
Another very important determinant of success is the general practitioner’s communication with the specialist. In this case, communication with my periodontist, Dr. Scott Froum, took place during telephone conversations, office visits, and even at the dinner table with models in hand! I generated a surgical index for him to follow (Figs. 2a, 2b, 2c) based on the diagnostic wax-up. We discussed opening the vertical dimension 2 mm, broadening her smile to reduce the negative space between her cheeks, restoring the appropriate length and width of the teeth, and the healing time needed prior to temporization and finalization.
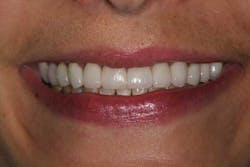
When all team members are on the same page and communication is established before the case is started, you put yourself in the position to create a superb result as was achieved in this case. (Figs. 3 and 3a)