Extraction/immediate implant placement with provisional for a patient with Guillain-Barré syndrome
Guillain-Barré syndrome (GBS) is a rare neurological autoimmune disorder that affects about one or two people each year within a population of 100,000.1 As a result of GBS, the body's immune system mistakenly attacks part of its peripheral nervous system—the network of nerves located outside of the brain and spinal cord. The severity of GBS can range from very mild, brief weakness to nearly devastating paralysis that leaves the individual unable to breathe independently.2
Depending upon the patient, GBS can present with symptoms that would interfere with certain types of dental treatment, such as procedures for which the patient would have to sit in the dental chair for prolonged periods of time or return for repeated appointments. Patients can experience weakness in the legs, arms, and body that sometimes spreads to the breathing muscles, face, and throat. Patients also commonly report painful tingling, a feeling of pins and needles, and numbness in addition to muscle pain. In more severe cases, patients may have difficulty swallowing and become breathless. Depending on the type of GBS, the patient’s pulse may be too rapid or too slow, and blood pressure may rise too high or fall too low.2 Fortunately, most people eventually recover from even the most severe cases of GBS.
Although treating a patient with GBS can be complex, a dental implant can provide for a better quality of life. The most challenging of the GBS symptoms for the dental professional is progressive weakness that can affect the muscles of the upper body and face, as well as some important masticatory muscles such as the buccinator or masseter.3 Replacement of missing teeth with dental implants can improve the chewing function in patients with GBS. However, any replacement of missing teeth by removable prosthesis is not recommended (as it may cause poor neuromuscular coordination during chewing, along with altered muscular movement patterns). Clinicians treating patients with GBS should consider fixed prosthesis treatment for rehabilitation of the fully or partially edentulous area.4
Case report
Case presentation
Treatment considerations
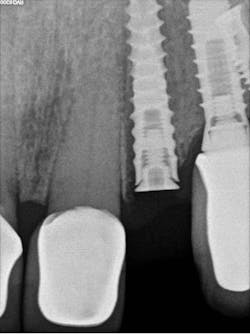
The decision to use the Ditron Implant System was based on the following treatment plan: extraction and immediate implant placement, with immediate provisionalization using a final titanium abutment. Extraction and immediate implant placement with immediate provisionalization have shown to be quite successful.
One retrospective study of 206 implants placed into fresh extraction sites using a flapless technique, followed by immediate provisionalization, showed cumulative survival and success rates of 98.77% (mean follow-up at 23.1 months).5 Another retrospective study of 100 cases concluded that immediate provisionalization of implants placed into fresh extraction sites can be effective even when minimal provisionalization criteria are met.6
Maintaining initial stability is important when an implant is placed in a compromised extraction site, since there is less bone-to-implant contact there than in a healed site. Because of its architecture, the Ditron Ultimate implant offers a very high initial stability and strong abutment connection. The implant profile uniformly distributes the stress directly to the bone, which results in a more even distribution of force and lower long-term crestal resorption. This implant system has a good aggressive thread profile and a secure abutment connection, which are both key characteristics. The microthreads on the implant’s reverse conical neck (RCN) greatly increase the implant’s ability to resist axial displacement, and the mechanical stimulus the microthreads provide helps to preserve the peri-implant marginal bone. By inserting an Ultimate implant, 5.57 mm3 of bone will be saved compared to that of a non-RCN implant.7
Clinical treatment
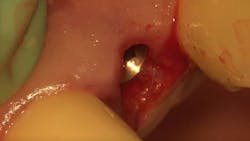
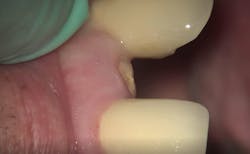
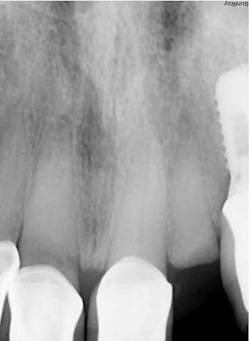
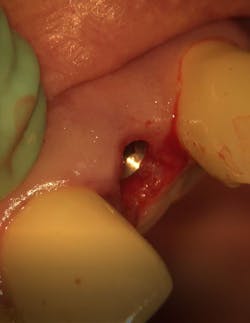
First visit: Extraction and immediate implant placement, immediate placement of the final abutment prepared intraorally, and then a provisional out of function.
Second visit: After two months of healing, final impressions were taken.
Third visit: The final crown was delivered.
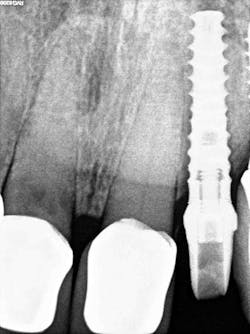
The implant was allowed to heal for two months before impressions were taken. The final zirconia crown was delivered two weeks later (figure 6).
Conclusion
With his previous implant tooth replacements, this patient had an arduous recovery. He experienced severe postsurgical pain and had to endure prolonged treatment time because of his challenging recovery. After this most recent implant placement, the patient reported to our office that he had absolutely no postoperative discomfort, no prosthesis complications, and he was very impressed by the entire experience. He reported that he did not need any postsurgicalThis case study shows that implant placement can be successful even in patients with difficult medical issues if the clinician adheres to the correct protocols and uses a precision implant system.
Clinical treatment by Robert J. Miller, DDS, and Technics Dental Laboratory
Disclosures or conflicts of interest: Dr. Miller is a clinical advisor for Ditron Dental USA. Products mentioned in this article are used in the regular course of practice.
References
- Guillain-Barré syndrome. National Organization for Rare Disorders. Updated 2020. https://rarediseases.org/rare-diseases/guillain-barre-syndrome/
- Guillain-Barré syndrome fact sheet: What is Guillain-Barré syndrome? National Institute of Neurological Disorders and Stroke. June 2018. Updated March 16, 2020. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-sheets/Guillain-Barr%C3%A9-Syndrome-Fact-Sheet
- van Doorn PA, Ruts L, Jacobs BC. Clinical features, pathogenesis, and treatment of Guillain‐Barré syndrome. Lancet Neurol. 2008;7(10):939‐950. doi:10.1016/S1474-4422(08)70215-1
- Faraji F, Bayani M, Jafarpour M, Abdolalian F. Maxillary sinus floor augmentation and simultaneous dental implant placement in a patient with Guillain-Barre syndrome: a case report. Clin Case Rep. 2019;7(12):2331-2335. doi:10.1002/ccr3.2485
- El-Chaar ES. Immediate placement and provisionalization of implant-supported, single-tooth restorations: a retrospective study. Int J Periodontics Restorative Dent. 2011;431(4):409-419.
- Becker CM, Wilson TG Jr, Jensen OT. Minimum criteria for immediate provisionalization of single-tooth dental implants in extraction sites: a 1-year retrospective study of 100 consecutive cases. J Oral Maxillofac Surg. 2011;69(2):491-497. doi:10.1016/j.joms.2010.10.024
- ULT™ Ultimate Precision Implant. Ditron Dental Molecular Precision Implant Systems. http://ditrondental.com/ultimate/
About the Author

Robert J. Miller, DDS
Robert J. Miller, DDS, graduated with honors from New York University College of Dentistry in 1981, where he received the International College of Dentists Award for clinical excellence, and then completed his residency at Flushing Medical Center in New York City. A board-certified diplomate of the American Board of Oral Implantology, Dr. Miller is a fellow of the American College of Dentists and the Academy of Osseointegration, an honored fellow of the American Academy of Implant Dentistry, a diplomate of the International Congress of Oral Implantologists, and acting chairman of the department of oral implantology at the Atlantic Coast Dental Research Clinic in Palm Beach, Florida. He is director of the Center for Advanced Aesthetic and Implant Dentistry in Delray Beach, Florida, and codirector of the Pacific Institute for Advanced Dental Education. Dr. Miller maintains a full-time practice dedicated to implant dentistry and revision surgery, has an active international lecture schedule, and is involved in biomaterial, laser, and dental implant research.