My dental implant screw loosened: Did I miss something?
Abstract
Dental implants are one of the go-to options to replace missing teeth. Like any other medical device, their longevity could be threatened by a complication. Screw loosening is one of the top complications impacting dental implants. This article will address two potential causes for this and possible solutions for achieving the proper preload.
Introduction
A number of options are available to replace missing or soon-to-be-missing teeth. Dental implants are often selected as the treatment of choice as they have historically demonstrated a high level of success1 and are well accepted by patients. While dental implants generally achieve a steady state of function, clinicians have seen that they are not without complications, as is the case with any medical device.2 Screw loosening is one of the more common complications, particularly with single-tooth implant-supported crowns, with a reported incidence of 5%–12% from 1.2–7 years.3,4
Reasons why the screw could be loose
There may be a variety of reasons why the screw that stabilizes the abutment to the implant might loosen.5 However, the overriding cause stems from the applied forces to the screw joint being greater than the clamping force. The phenomenon, known as preload, occurs when the screw is tightened within its elastic limits and optimizes the abutment-implant joint to hold steady.6
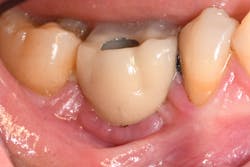
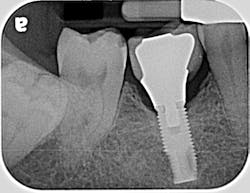
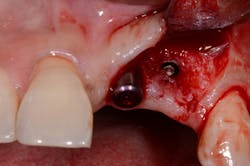
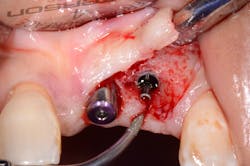
If the occlusal forces delivered to the implant-abutment-crown complex exceed the screw’s clamping ability, this may result in either its loosening (figures 1a and 1b) or, in more severe situations, fracturing of the screw (figures 2a–2c). Clinicians often indite the occlusion as being the primary culprit for the problem; however, in a number of instances, this may not be the case. The cause of screw loosening could also be due to using aftermarket parts, which do not have the precise fit of those made by the manufacturer of the implant.7
Another possible source of the problem may be the torque driver used to tighten the screw to achieve the proper preload target torque. Dental implant torque tools are designed to assist the clinician in reaching the targeted torque value for optimal preload. The issue with torque drivers is that with repeated use and sterilization, their markings may become difficult to read (figure 3).
This can be especially true with those of the beam type, which also happen to be the most popular. Moreover, when in clinical use, the clinician often swings the beam and visualizes the numbers from an angle rather than directly (figures 4a–4c).
This may cause the clinician to misread the actual value due to parallax. While the correct value (figure 5a) may have been achieved, in actuality it is perceived as being too high (figure 5b) or too low (figure 5c).
Parallax relates to objects appearing different based on the position from which they are viewed. For example, in the maxilla, when the beam is swung away from the clinician, the viewer’s angle may lead one to believe that the arm is at the center of the value when in fact it is below the desired total torque. The opposite would be true of the mandible when the beam swings toward the clinician; the actual value would be below what is desired. This deviation can be quite significant, especially if the ultimate torque for some abutment screws is 15 N-cm.
Over- or underreading the value could lead to a 20% error, which is way beyond the permissible 6% deviation allowed by ISO 6789.8 If under the ideal value, the screw may loosen, causing micromotion or mobility of the abutment, and allow potential particulate titanium material to get into the tissue, which can cause a foreign body reaction9 or, worse, fracture of the screw or even the implant. If the value exceeds the ideal torque, deformation of the screw beyond its plastic limits may result, which again would affect preload leading to screw loosening.
Solutions for achieving proper preload
Our torque drivers in dentistry carry a similar function as those used by many industries outside the profession. Your car’s tires and the various parts of an airplane all rely on torque-driven security. These various torque devices are all governed in their use and maintenance by the International Organization for Standardization (ISO). The same standard known as ISO 6789 is applied to all torque-limiting devices and states that torque-setting devices must be checked for calibration at least annually or more frequently.8 This is especially true if subjected to nonambient temperatures used during the sterilization process or even during storage. If the broken-arm-type torque drive is not carefully cared for, the spring could be adversely impacted or particulate debris could accumulate, leading to diminished accuracy. It is the clinician’s obligation to regularly follow through in checking the calibration of his/her torque drivers.
With regard to the issue of parallax, a device is available that can help avoid this error. The Beam Easy True Torque Reader (BETTr) is a simple device inserted into the scale of the beam. The clinician can establish a preset for the desired ultimate value. Once the beam reaches this value, it will begin to be displaced, indicating that the proper value has been reached (figure 6).
The alternative method is to set the BETTr device to zero on the scale and then swing the beam to the desired value. The clinician can check the value reached to make sure it is correct. If it isn’t, further correction should be made to set the screw properly.
Conclusion
This article explores two causes to possible screw loosening that have not been adequately assessed or addressed in the literature. It is the goal for any innovative device to be simple to use and provide meaningful benefit to our patients’ treatment outcomes. The exploration for improving upon our dental implant treatment will continue for all phases of care. Improving on the care and use of torque drivers can only help to improve our long-term treatment of patients by providing a more predictable, steady state for implants and their restorations.
Editor’s note: This article originally appeared in Perio-Implant Advisory, a chairside resource for dentists and hygienists that focuses on periodontal- and implant-related issues. Read more articles and subscribe to the newsletter.
References
- Adell R, Eriksson B, Lekholm U, Brånemark P-I, Jemt T. A long-term follow up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxiollfac Implants. 1990;5(4):347-359.
- Froum SJ, ed. Dental Implant Complications: Etiology, Prevention, and Treatment. 2nd ed. Wiley-Blackwell; 2015.
- Goodacre BJ, Goodacre SE, Goodacre CJ. Prosthetic complications with implant prostheses (2001-2017). Eur J Oral Implantol. 2018;11(Suppl 1):S27-S36.
- Katsavochristou A, Koumoulis D. Incidence of abutment screw failure of single or splinted implant prostheses: a review and update on current clinical status. J Oral Rehabil. 2019;46(8):776-786. doi:10.1111/joor.12817
- Nithyapriya S, Ramesh AS, Kirubakaran A, Mani J, Raghunathan J. Systematic analysis of factors that cause loss of preload in dental implants. J Indian Prosthodont Soc. 2018;18(3):189-195. doi:10.4103/jips.jips_294_17
- Hurson S. Use of authentic, integrated dental implant components vital to predictability and successful long-term clinical outcomes. Compend Contin Educ Dent. 2016;37(7):450-455.
- Gigandet M, Bigolin G, Faoro F, Bürgin W, Brägger U. Implants with original and non-original abutment connections. Clin Implant Dent Relat Res. 2014;16(2):303-311. doi:10.1111/j.1708-8208.2012.00479.x
- ISO 6789-1:2017. Assembly tools for screws and nuts – hand torque tools – Part 1: Requirements and methods for design conformance testing and quality conformance testing: minimum requirements for declaration of conformance. International Organization for Standardization. February 2017. https://www.iso.org/standard/62549.html
- Fretwurst T, Nelson K, Tarnow DP, Wang HL, Giannobile WV. Is metal particle release associated with peri-implant bone destruction? An emerging concept. J Dent Res. 2018;97(3):259-265. doi:10.1177/0022034517740560
About the Author

Paul S. Rosen, DMD, MS
Paul S. Rosen, DMD, MS, maintains private practices limited to periodontics and dental implants in Yardley, Pennsylvania, and New York, New York. He is a clinical professor in the department of periodontics at the University of Maryland School of Dentistry in Baltimore, Maryland. He is also an adjunct professor at the James Cook University Dental School College of Medicine and Dentistry in Cairns, Queensland, Australia.